 |
 |
| Korean J Anesthesiol > Volume 75(6); 2022 > Article |
|
In this case-based technical report, the novel and straightforward obturator fascia compartment (OFC) block will be described. This superficial fascial block targets the pudendal nerve (PN) at the level of AlcockŌĆÖs canal and, ultimately, the nerve to the obturator internus (NOI). Owing to the cranial spread of the local anesthetic below the obturator fascia, the OFC block can potentially anesthetize the proximal rami of the PN (Fig. 1AŌĆōC). Written informed consent for publication was obtained from the patient.
Fig. 1A and 1B show shows a 66-year-old patient who underwent a vulvectomy in the context of oncologic disease and experienced intense pain in the post-anesthetic care unit despite receiving significant intravenous (IV) analgesia (8 mg IV morphine, 1 g IV paracetamol, 2 g IV metamizol, 30 mg IV ketorolac, 2 g IV magnesium sulfate, 15 mg IV ketamine, and 150 mg IV tramadol). After the block, immediate pain relief was achieved (the pre-block numeric pain rating scale score was 9 out of 10). Under conventional analgesia (1 g IV paracetamol every 8 h, 2 g IV metamizol every 12 h, 100 mg IV tramadol every 8 h, and IV ketorolac 30 mg every 8 h), the patient had a numeric pain rating scale score < 2 starting on postoperative day one. The patient reported numbness and thermally sensitive alterations in the perineal region for 12 h (8 ml of ropivacaine 0.5% were given per side).
For the OFC block, the patient is placed in the lateral decubitus position with the hips flexed at 90┬░. After observing the ischial tuberosity (IT) with the probe positioned transversally but oriented cranially (towards the patientŌĆÖs head), the sacrotuberous ligament (STL) is visualized covering the IT medially at the inferior edge (thinner portion) of the gluteus maximus superficial to the ligament (the STL runs from the IT to its medial/upper insertion in the sacrum). Unlike with other approaches at the obturator foramen level, in this view, the gemelli muscles are not observed and are thus not a complicating factor (Fig. 1AŌĆōC).
The needle is then inserted from the lateral side in the vicinity of the IT and advanced in the caudal to cranial direction, targeting the medial/superior surface of the Obturator Internus Muscle (OIM). It is advanced tangentially to the superficial (distal) third of the STL. This maneuver facilitates local anesthetic spread beneath the obturator fascia, which can be seen running deeply and cranially (the OIM is visualized in the short axis view below the STL). On ultrasound, the local anesthetic can be seen dispersing easily within AlcockŌĆÖs canal owing to the textile arrangement of its walls (a single layer of the obturator fascia) (Fig. 1A and 1B).
Owing to the proximal emergence of the inferior rectal nerve, a proximal PN block is necessary for proctologic procedures. While transperineal techniques reach the branches to the genitals, such as the dorsal penis/clitoris or dorsal labial nerves, they spare the inferior rectal nerves and several perineal nerve rami. The transvaginal techniques, on the other hand, only uses landmarks as guidance and may cause discomfort and ultimately fail [1].
The proximal ultrasound-guided technique at the level of the ischial spine relies on the accurate identification of the ischial spine and the sacrospinous ligament (SSL) (deep structures) immediately caudal to the piriform muscle and cranial to the OIM. Though the injection is performed only after the neurovascular structures are identified, intrapelvic organs can easily be inadvertently punctured given the lack of muscular layers beneath the SSL [1].
Bendtsen et al. [1] have previously described a PN block at the entrance of AlcockŌĆÖs canal that can anesthetize all three branches of the PN before they ramify in the ischioanal fossa. The roadmap described by these authors suggests that the PN can be targeted at this level by following the margin of the hip bone sonographically (cranial to caudal direction) along the 1) greater sciatic notch, 2) ischial spine, and 3) lesser sciatic notch. However, this technique requires maneuvering in the deep, thick, and round gluteal region where minor probe adjustments can cause dramatic changes in the ultrasound image.
To the best of my knowledge, a PN block at the obturator foramen level has only been described in cadaveric specimens. For this block, the PN is approached from the lateral side (which eliminates the need to cross the ischiorectal fossa); however, this technique still requires a perineural injection around milimetric structures within AlcockŌĆÖs canal [2]. Some difficulties with this approach include identifying the OIM and obturator fascia beneath the thick gluteus maximus and the need to place the patient in the prone position [2].
The OIM belongs to the external hip rotator muscle group. It is the only component that posteriorly covers the obturator foramen (the superior and inferior gemelli muscles arise from the posterior surface of the superior ramus of the ischium and run laterally) [3].
The obturator fascia splits to form AlcockŌĆÖs canal, which encloses the pudendal vessels and the PN when they cross over the surface of the OIM. Of note, the obturator fascia attaches distally to the STL [4,5]. Fortunately, anesthesia of the PN can be achieved without the need to identify AlcockŌĆÖs canal, which can be visualized easier on ultrasound after an OFC block. However, the PN anatomy has considerable variability and thus the OFC block is a tool that increases the success of and democratizes the PN block [4,5] by reducing the prevalence of unsuccessful injections in the ischiorectal fossa in the vicinity of AlcockŌĆÖs canal (Fig. 1AŌĆōC).
However, the pudendal block is ineffective in the transobturator tape (TOT) procedure for female urinary incontinence, as the cranial portion of the vagina is innervated by the uterovaginal nerves from the hypogastric plexus; nevertheless, the afferences, through the NOI, from the obturator fascia and the OIM (both crossed by the TOT) are a source of postoperative pain that can be managed using the OFC block.
Therefore, the OFC block may be helpful in adult and pediatric patients undergoing urologic, proctologic, and gynecologic/obstetric surgeries.
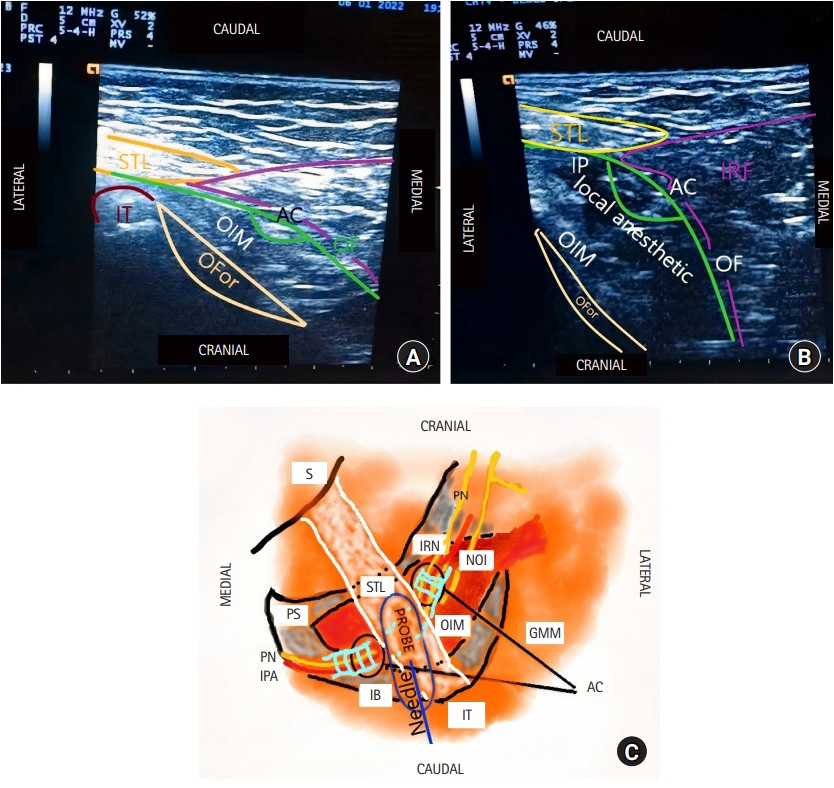
Fig.┬Ā1.
(A) Ultrasound image showing the relevant sonoanatomy for performing the OFC block with the relevant structures identified, (B) Ultrasound image showing the OFC block injection. The local anesthetic is injected superficially beneath the obturator fascia. It then spreads cranially and penetrates AlcockŌĆÖs canal, spreading its contents. In this image, AlcockŌĆÖs canal is visualized in its oblique/long axis. After the injection, it is easier to effectively and clearly visualize AlcockŌĆÖs canal and its contents (pudendal nerve, pudendal vessels), (C) Schematic image showing the relevant anatomy for the OFC block. The needle is advanced in the caudal to cranial direction. The obturator fascia is not represented. It covers the obturator internus muscle medially/posteriorly. IT: ischial tuberosity, AC: AlcockŌĆÖs canal, OF: obturator fascia, OIM: obturator internus muscle, IP: injection point, OFor: obturator foramen, IRF: ischiorectal fossa, IRN: inferior rectal nerve, PN: pudendal nerve, S: sacrum, PS: pubic symphysis, NOI: nerve to the obturator internus, IB: ischial bone, STL: sacrotuberous ligament, IPA: internal pudendal artery, GMM: gluteus maximus muscle.
References
1. Bendtsen TF, Parras T, Moriggl B, Chan V, Lundby L, Buntzen S, et al. Ultrasound-guided pudendal nerve block at the entrance of the pudendal (Alcock) canal: description of anatomy and clinical technique. Reg Anesth Pain Med 2016; 41: 140-5.


2. Soucy B, Luong DH, Michaud J, Boudier-Rev├®ret M, Sobczak S. Accuracy of ultrasound-guided pudendal nerve block in the ischial spine and AlcockŌĆÖs canal levels: a cadaveric study. Pain Med 2020; 21: 2692-8.



3. Solomon LB, Lee YC, Callary SA, Beck M, Howie DW. Anatomy of piriformis, obturator internus and obturator externus: implications for the posterior surgical approach to the hip. J Bone Joint Surg Br 2010; 92: 1317-24.











