 |
 |
| Korean J Anesthesiol > Volume 77(1); 2024 > Article |
|
Abstract
Background
Methods
Results
NOTES
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
Author Contributions
Insun Park (Conceptualization; Data curation; Formal analysis; Investigation; Methodology; Project administration; Resources; Software; Validation; Visualization; Writing – original draft)
Seukyoung Hong (Data curation)
Su Yeon Kim (Data curation; Formal analysis)
Jung-Won Hwang (Conceptualization; Project administration; Writing – review & editing)
Sang-Hwan Do (Conceptualization; Supervision; Validation; Writing – review & editing)
Hyo-Seok Na (Conceptualization; Investigation; Methodology; Project administration; Resources; Software; Supervision; Validation; Visualization; Writing – review & editing)
Fig. 1.
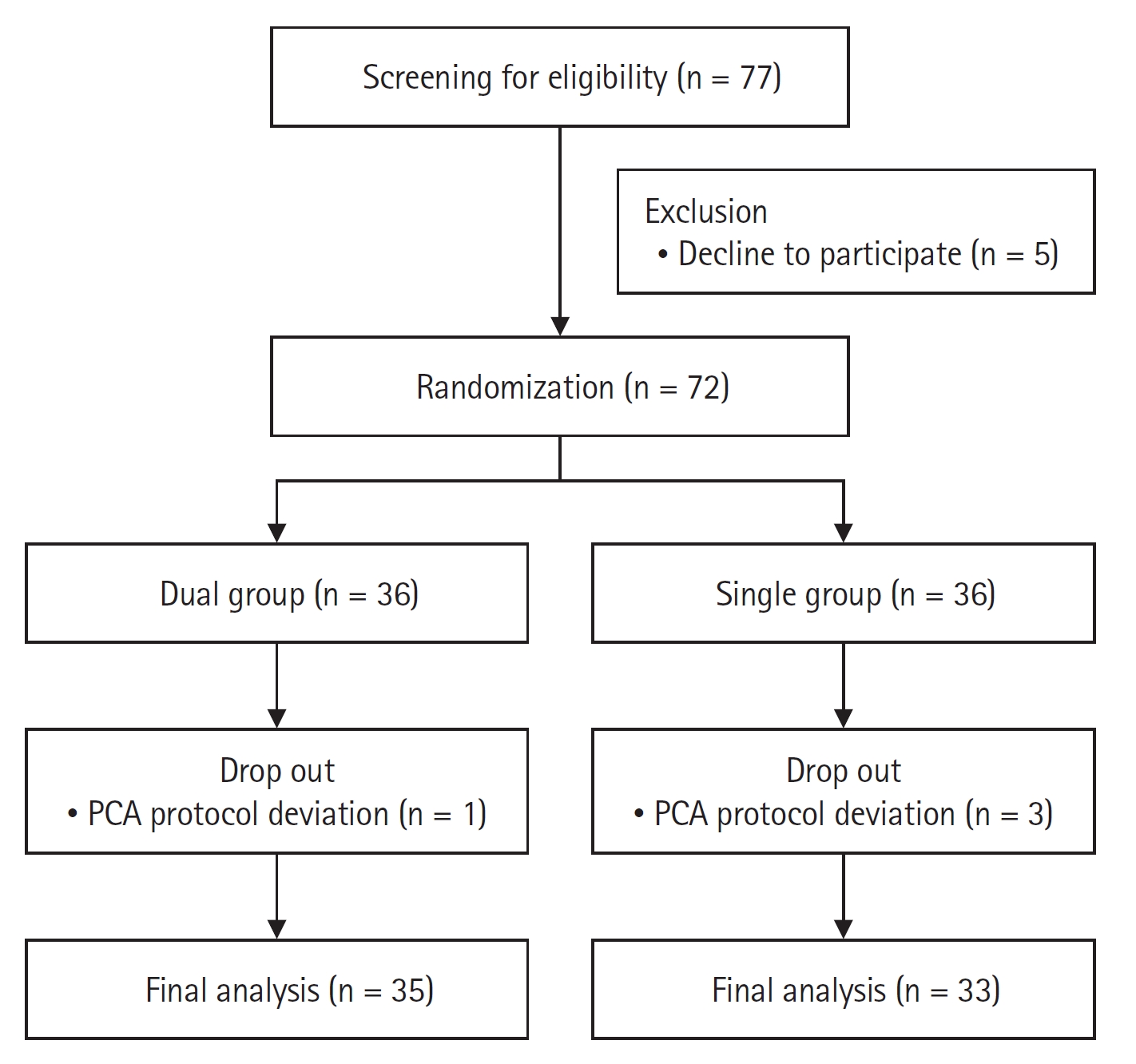
Fig. 2.
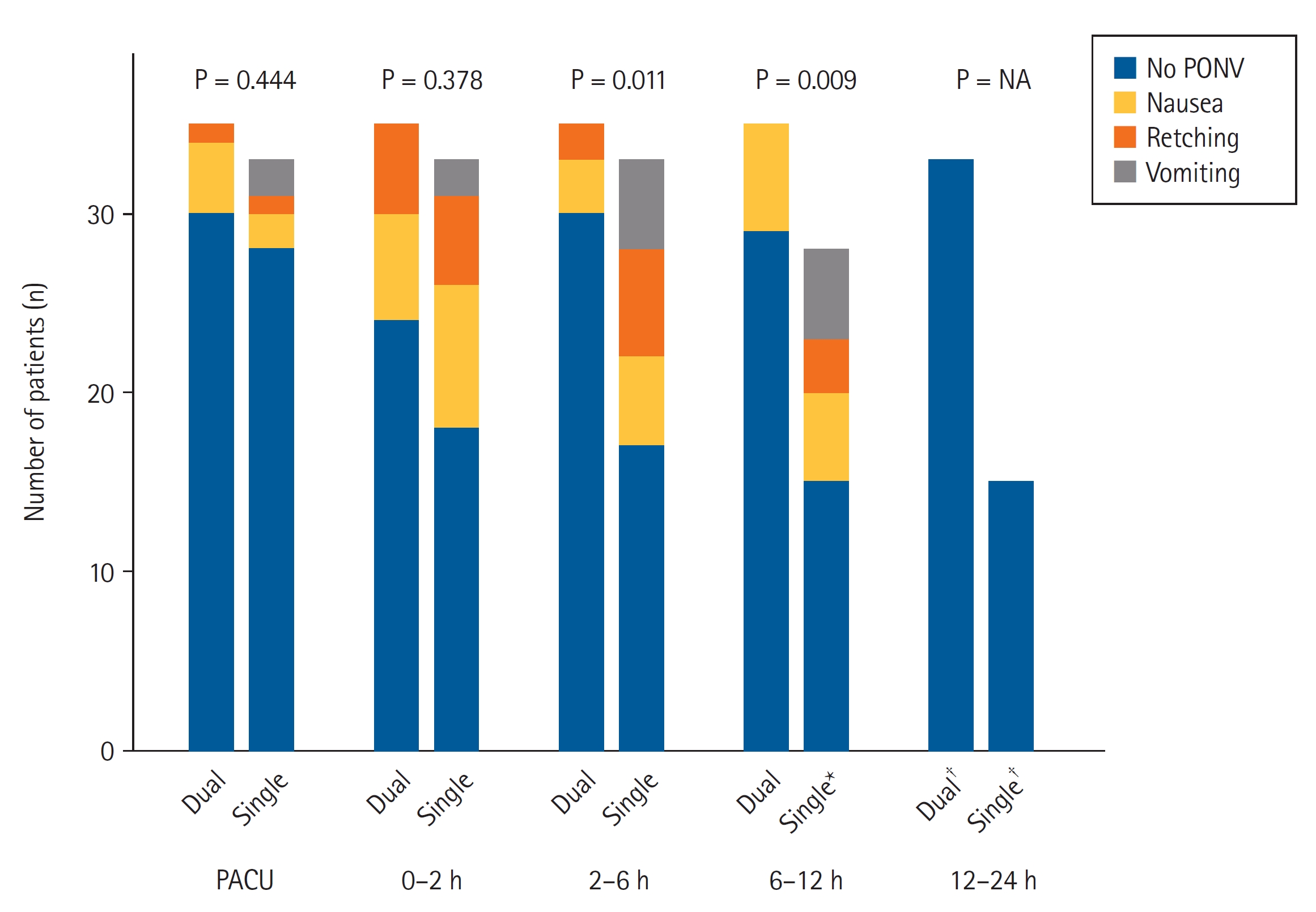
Fig. 3.
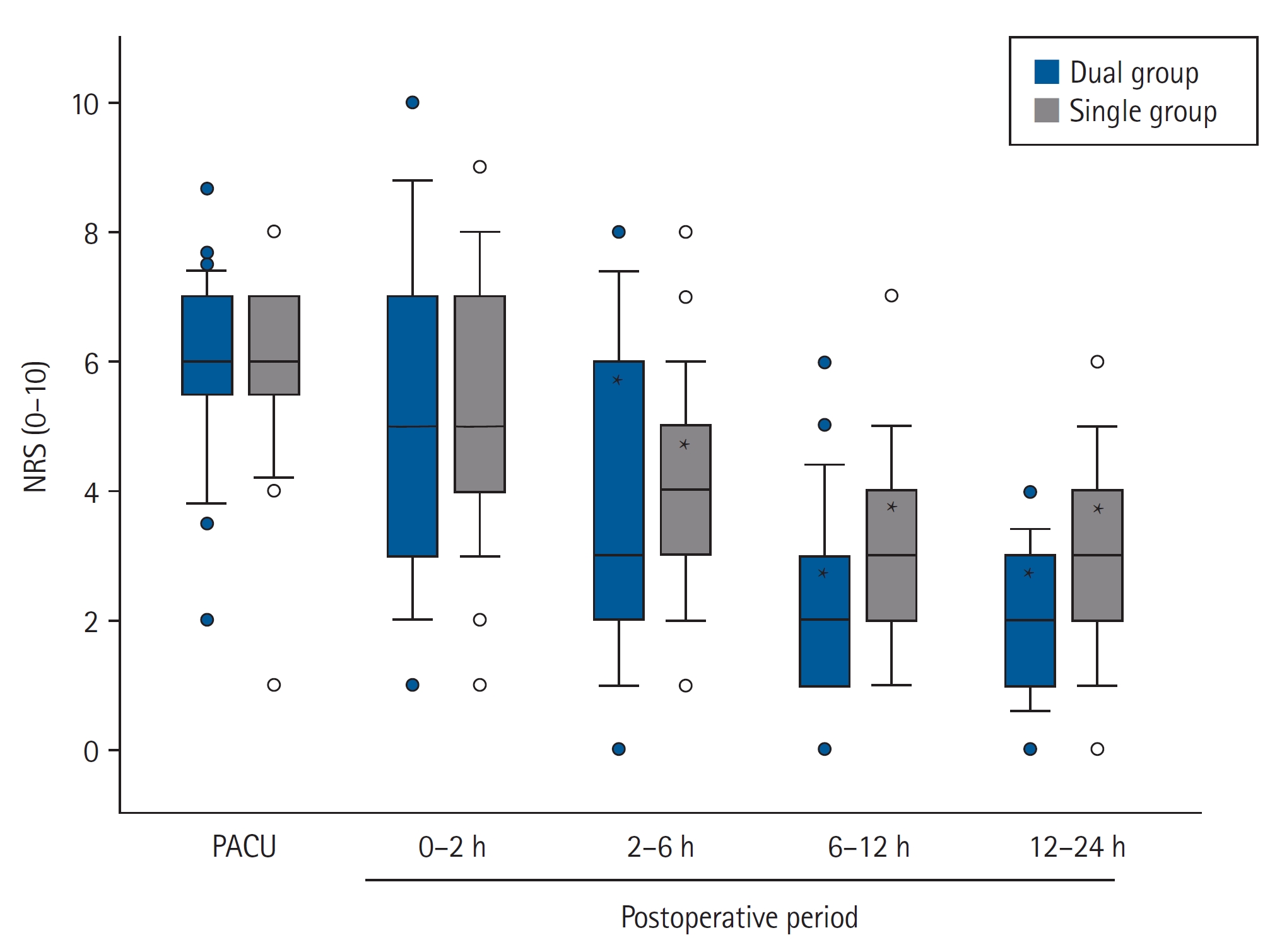
Table 1.
Values are presented as mean ± SD or number (%). Dual group: ketorolac and fentanyl delivered by a dual-chamber PCA, Single group: fentanyl alone delievered by a PCA. ASA PS: American Society of Anesthesiologists physical status, PONV: postoperative nausea and vomiting, SBP: systolic blood pressure, DBP: diastolic blood pressure, HR: heart rate, PACU: post-anesthesia care unit.
Table 2.
| Time | Dual group (n = 35) | Single group (n = 33) | P value |
|---|---|---|---|
| 0–2 h | 22 (62.9) | 26 (78.8) | 0.150 |
| 2–6 h | 13 (37.1) | 19 (57.6) | 0.092 |
| 6–12 h | 8 (22.9) | 10 (30.3) | 0.487 |
| 12–24 h | 3 (8.6) | 8 (24.2) | 0.079 |









