 |
 |
| Korean J Anesthesiol > Volume 77(1); 2024 > Article |
|
Abstract
Background
Methods
Results
NOTES
Data Availability
The authors have placed an embargo on the public availability of the data due to ongoing secondary analyses.
Author Contributions
Hui Ju (Data curation; Formal analysis; Investigation; Methodology; Project administration; Resources; Software; Validation; Writing – original draft; Writing – review & editing)
Kai Shen (Data curation; Resources; Supervision)
Jiaxin Li (Formal analysis; Writing – original draft)
Yi Feng (Conceptualization)
Fig. 1.
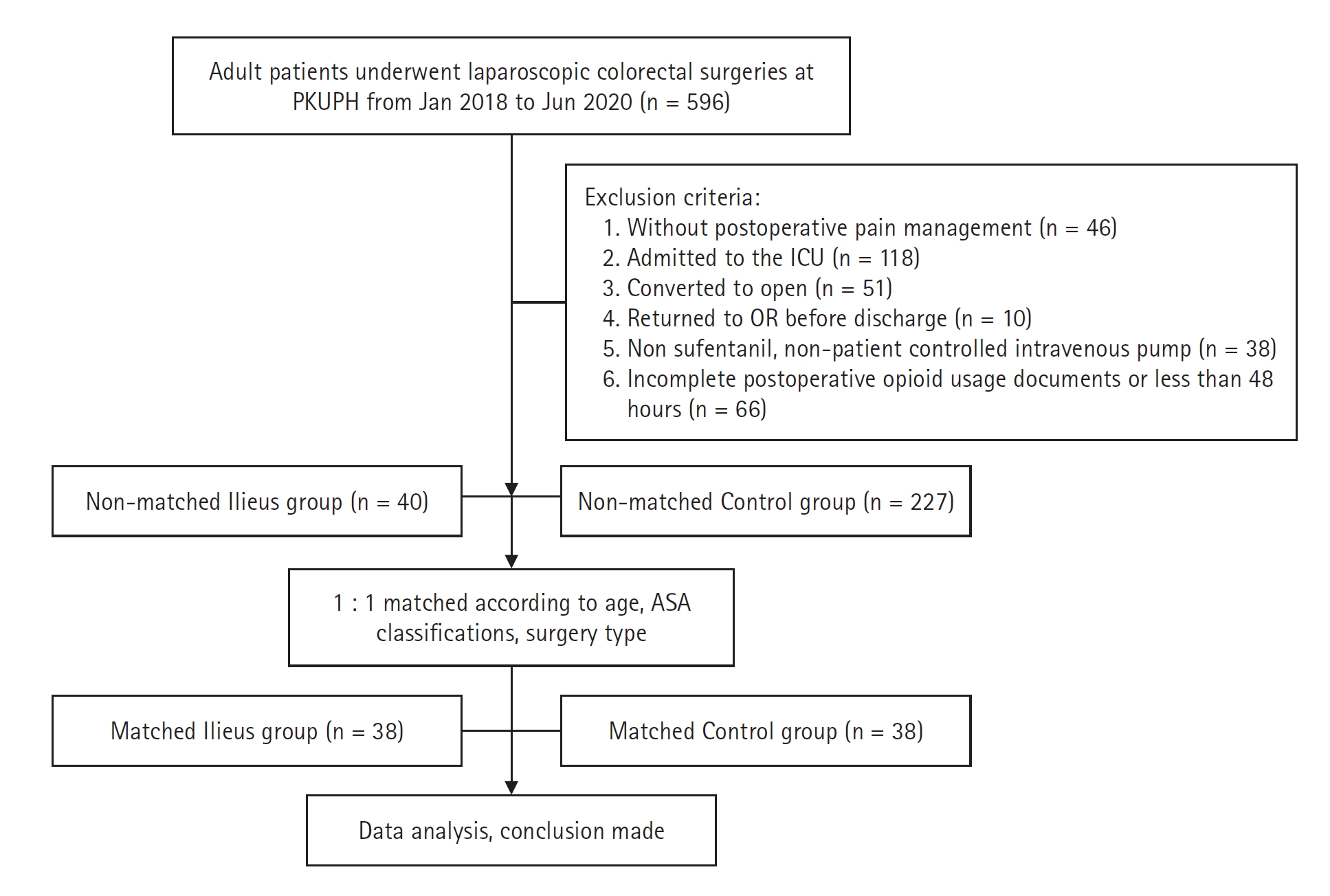
Table 1.
Values are presented as mean ± SD, number (%) or median (Q1, Q3). ASA PS: American Society of Anesthesiologists physical status, TAP: transversus abdominis plane, TPOD: total postoperative opioid dose, PCA: patient-controlled analgesia, POD: postoperative day, DoHS: duration of hospital stay. *Intraoperative opioids were converted to equivalent doses of morphine (mg/kg).









