Laser enucleation and morcellation of the prostate is increasingly used for the surgical management of bladder outflow obstruction. It is an effective and safe surgical procedure for treating symptomatic benign prostatic hyperplasia (BPH) and is associated with low morbidity and short hospital stay [1]. As a result of the excellent hemostatic properties of the holmium wavelength and the use of iso-osmotic saline as the irrigating solution, the transfusion rate is minimal and transurethral resection syndrome rarely occurs [2]. However, it can be associated with several morbidities, including capsular perforation, as well as ureteral orifice and bladder mucosal injuries [3]. We report a case of severe postoperative dyspnea caused by neglected massive intraperitoneal fluid collection during laser enucleation and morcellation of the prostate.
Case Report
A 79-year-old male patient was scheduled for holmium laser enucleation and morcellation of the prostate to treat BPH. He exhibited acute obstructive symptoms of the lower urinary tract and gross hematuria. His weight and height were 59.7 kg and 166.5 cm. He was previously healthy and had no other medical history. Preoperative laboratory findings and chest X-ray findings were within normal ranges. Preoperative electrocardiography showed a normal sinus rhythm, and echocardiography showed normal left ventricular function. The volume of the prostate gland, measured preoperatively using endorectal ultrasonography, was 98 ml, including 75 ml for the transitional zone of the prostate.
Upon arrival at the operating room, his systolic/diastolic blood pressure was 120/90 mmHg, heart rate was 70 bpm, and peripheral oxygen saturation was 99%. Routine monitoring was conducted such as electrocardiography, peripheral oxygen saturation, non-invasive blood pressure, end-tidal carbon dioxide, and body temperature. Anesthesia was induced with 250 mg of sodium thiopental, 50 mg of rocuronium, and sevoflurane, and was maintained with sevoflurane (2ŌĆō3 vol%), N2O (1 L/min), and oxygen (1 L/min), with supplemental rocuronium. Continuous arterial blood pressure was monitored via the left radial artery using a 20 G catheter. Initial arterial blood gas analysis in 50% oxygen showed values of pH 7.42, arterial partial pressure of carbon dioxide (PaCO2) 44 mmHg, arterial partial pressure of oxygen (PaO2) 245 mmHg, bicarbonate (HCO3ŌĆō) 28.5 mEq/L, base excess 3.4, Na+ 141 mEq/L, K+ 3.7 mEq/L, and hematocrit 40%.
Following repeated massive bladder irrigation with saline, ~150 ml of blood clots were evacuated using an Ellik evacuator and the bladder distension was relieved immediately. Next, holmium laser enucleation and morcellation of the prostate was initiated using an isotonic saline solution for bladder irrigation. At this moment, his vital signs showed a systolic/diastolic blood pressure of approximately 130/80 mmHg, heart rate of 85 bpm, and oxygen saturation at 100%. Peak airway pressure was 11 cmH2O. One hour after the beginning of the procedure, the peak airway pressure increased to 23 cmH2O. On auscultation, the lung sounds were clear. At the end of the surgery, it reached 28 cmH2O. However, oxygen saturation was maintained at 99%. No significant hemodynamic changes developed during the surgical procedure, and estimated blood loss was less than 100 ml. The total operation time was approximately 110 min. During the operation, a total of 45000 ml of saline was used for bladder irrigation. After completion of the procedure, 2 mg of neostigmine and 0.4 mg of glycopyrrolate for neuromuscular blockade reversal were administered intravenously. The patient was extubated after recovery from neuromuscular blockade, which was confirmed by hand grip and head lift.
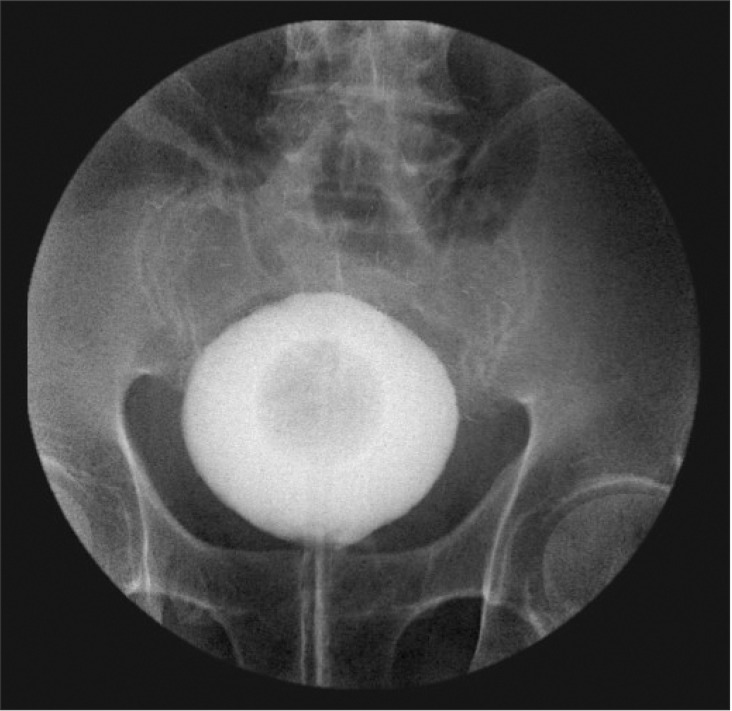
Immediately after tracheal extubation, he experienced severe respiratory difficulty with low SpO2 (~90%) and complained of severe abdominal pain. Physical examination revealed a tense and distended abdomen. The patient's systolic/diastolic blood pressure was 110/85 mmHg with heart rate of 95 bpm. After applying a 100% O2 mask, arterial blood gas analysis indicated values of pH 7.15, PaCO2 56 mmHg, PaO2 72 mmHg, HCO3ŌĆō 20 mEq/L, base excess -9.7, Na+ 144 mEq/L, K+ 3.8 mEq/L, and hematocrit 38%. He was re-intubated using 5 mg of midazolam and 30 mg of rocuronium, and his peak airway pressure was 25 cmH2O at this time. Chest X-ray showed acute pulmonary venous congestion and subsegmental atelectasis in both lower lobes. He received 20 mg of furosemide intravenously. The cystogram showed no leakage of contrast media (Fig. 1). An urgent computed tomography (CT) scan of the abdomen and pelvis was performed without tracheal extubation. The CT scan showed massive fluid collection in the abdominal pelvic cavity suggesting bladder wall injury but with no demonstrable discontinuity of the bladder wall (Fig. 2). To relieve intraperitoneal fluid collection, ultrasonography-guided aspiration was performed without complications (Fig. 3) and approximately 270 ml of fluid was drained.
The patient was transferred to the intensive care unit (ICU) and was closely monitored. Ultrasonography-guided aspiration was repeated and 320 ml of fluid was drained. Physical examination revealed a soft abdomen. Six hours after arrival at the ICU, careful extubation was performed. His systolic/diastolic blood pressure remained stable, around at 110/60 mmHg, with heart rate of 70 bpm. Urinary output was maintained at 80ŌĆō100 ml/h after ICU admission without renal impairment. The patient recovered uneventfully and was discharged on postoperative day 2.
Discussion
Laser enucleation and morcellation of the prostate has several advantages over standard transurethral resection of the prostate (TURP) including no upper limit in size for prostate removal [4], less bleeding risk than TURP, and short length of hospital stay [5]. With many advantages, laser enucleation and morcellation of prostate surgery has been replacing conventional TURP. However, laser enucleation and morcellation of the prostate has several disadvantages. Compared to other transurethral surgeries, significantly more tissue is extirpated, the surgical duration is longer, and the incidence of bladder injury is higher with enucleation and morcellation of the prostate [6]. The pooled result of a large case series revealed that enucleation and morcellation of the prostate can result in several complications including bladder neck false passage, capsular perforation, ureteral orifice injury, and bladder mucosal morcellation injury [3,7].
Classically, bladder perforation has been classified into intraperitoneal or extraperitoneal perforation from a urological perspective. Extraperitoneal perforation is more common than intraperitoneal perforation but is usually associated with a less severe clinical manifestation [8]. It can be relieved by conservative treatment, without surgical repair. However, intraperitoneal perforation is more serious and may be complicated by systemic absorption of irrigating solution [7,9]. Intraperitoneal perforation may also result in a significant increase in intraabdominal fluid with a subsequent increase in abdominal pressure. The resulting abdominal compartment syndrome causes several problems, including deterioration of ventilation, renal dysfunction, and reduction of perfusion to the abdominal organs [10]. Thus, intraperitoneal perforation is usually resolved by surgical treatment.
During laser enucleation and morcellation of the prostate, the enucleation procedure may thin or even perforate the prostatic capsule, leading to significant extraperitoneal accumulation of irrigation fluid [3]. Furthermore, the morcellation procedure may unintentionally involve the bladder mucosa or full-thickness bladder, eventually resulting in excessive bleeding, bladder perforation, intraperitoneal irrigant extravasation, or significant hemodynamic instability [3]. Thus, anesthesiologists should consider the possibilities of both intraperitoneal and extraperitoneal bladder perforation during laser enucleation and morcellation of the prostate.
In our case, generalized massive abdominal distension corresponds more with intraperitoneal bladder perforation rather than extraperitoneal perforation. Extraperitoneal bladder perforation is usually accompanied by tenderness and swelling of suprapubic and perineal area. Interestingly, cystogram and CT scan of the abdomen and pelvis did not reveal any contrast leakage or bladder wall discontinuity in this patient, even though they are the diagnostic standard of bladder rupture. It could be explained by well aligned injury of the bladder wall or blocked wound orifice by hematoma. In addition, a tiny bladder wall defect, which could not be detected by the CT scan, might have occurred during the surgical procedure. Fluid leakage via the tearing site could have sustained during the operation and paradoxically, increased intraabdominal pressure by fluid accumulation may have prohibited contrast dye leakage during cystogram. Although the patient exhibited massive fluid collection on the abdominal pelvic CT scan, he had a stable hemodynamic status and the abdominal distension was relieved by following ultrasonography-guided percutaneous drainage. He showed no significant intraabdominal organ dysfunction including renal failure. Therefore, we decided upon a conservative treatment rather than surgical repair. This case is worthy of note in that the radiologic images did not reveal definite bladder wall discontinuity and his clinical course was relatively less severe.
An important concern regarding the perioperative anesthetic management must be addressed. In this case, we neglected the continuous increase in peak airway pressure during the surgical procedure. It could be an early sign of increased intraabdominal pressure. We regret not performing a careful abdominal physical examination during the surgery and upon tracheal extubation. Although CT scan showed negative finding for definite bladder wall perforation, massive fluid collection in the abdominal pelvic cavity was a sign of bladder wall injury, which underscores the importance of monitoring physical signs of patients. Differential diagnosis of increased airway pressure must have taken place, by confirming the depth of endotracheal tube to rule out endobronchial intubation and suctioning the endotracheal tube. In addition, we regret not having performed additional laboratory tests such as arterial blood gas analysis, radiologic workup such as chest X-ray, and direct communication with the surgeon during the procedure. These neglected managements would have been helpful to avoid an unnecessary re-intubation and difficult postoperative care in this patient.
The current report describes severe postoperative dyspnea caused by neglected massive intraperitoneal fluid collection during laser enucleation and morcellation of the prostate. Although hemodynamic and respiratory parameters are monitored generally stable during the laser surgery of the prostate, anesthesiologists should always be aware of negligible changes of patient status which might be associated with infrequent surgical complications. Early detection and meticulous physical examination are always requisite to prevent progression to severe complications.