Association of HLA-DPA1 polymorphism with prolonged mechanical ventilation in patients undergoing liver transplantation
Article information
Abstract
Background
Prolonged mechanical ventilation (PMV) is a common complication after liver transplantation surgery. However, owing to the clinical and economic benefits of early extubation, many efforts have been used to assess the clinical predictors for PMV. The aim of our study was to explore the impact of perioperative risk factors, including candidate gene polymorphisms, for PMV in patients undergoing liver transplantation.
Methods
One hundred forty patients who underwent liver transplantation surgery were enrolled. The duration of mechanical ventilation after surgery was examined, along with the length of intensive care unit and hospital stay, and 30-day mortality. Patient-related clinical factors and single nucleotide polymorphisms of candidate genes were assessed with regard to PMV, which was defined as mechanical ventilation for > 48 h.
Results
Twenty-six (19%) patients continued to receive mechanical ventilation at 48 h after surgery. Intraoperative continuous renal replacement therapy (CRRT) and an elevated serum lactate level during the postoperative period were significantly associated with the PMV group, compared to the non-PMV group (odds ratio [OR] = 24.731 [1.077, 567.915] versus OR = 3.008 [1.497, 6.045]). A significant association existed between the HLA-DPA1 rs8486 polymorphism and the risk of PMV under the allele model (OR = 8.060 [1.451, 44.765]).
Conclusions
The rs8486 polymorphism in HLA-DPA1 can independently affect the risk of PMV in liver transplantation recipients, along with intraoperative CRRT application, and elevated lactate level during the postoperative period.
Introduction
Preoperative comorbidities, challenging surgical procedures, and complex postoperative management are the factors that make enhanced recovery after surgery difficult for liver transplantation patients. Early weaning from mechanical ventilation alleviates pulmonary complications such as atelectasis, intrapulmonary shunting, and pneumonia, and effectively improves patients’ recovery [1]. For graft survival matter, immediate extubation effectively promotes venous return to the heart and increases cardiac output and hepatic arterial blood flow, thereby helping to improve early graft function [2]. However, despite the clinical strength of early weaning from mechanical ventilation, identifying patients who are likely to receive prolonged mechanical ventilation (PMV) remains very difficult [3].
Patients undergoing PMV represent up to 15% of all patients requiring weaning from mechanical ventilation [4]. Patients who undergo PMV often have advanced chronic respiratory failure and/or other comorbidities, and eventually account for longer intensive care unit (ICU) stays and greater financial burden. Thus, emerging interests focusing on reducing the need for PMV and on predicting candidate patients who are at risk for developing PMV are needed. In 2005, a consensus conference led by the National Association for Medical Direction of Respiratory Care (NAMDRC) defined PMV as mechanical ventilation for ≥ 21 consecutive days for ≥ 6 h/days with invasive (i.e., via endotracheal tube or tracheostomy) and/or noninvasive (i.e., facial/nasal interface) methods of delivery [5]. However, a great diversity exists in the definition of PMV in many published studies [6-10]. In most critical care and postoperative patient management-based studies, PMV has been variously defined as duration of mechanical ventilation of > 24 h [6], > 48 h [7], > 14 days [8], to as long as > 29 days [9], or as the need for mechanical ventilator support during post-ICU care [10].
Various studies have identified patient-related clinical factors that contribute to the development of PMV such as an excessive amount of red blood cells or fresh frozen plasma transfusion, low preoperative platelet count (i.e., < 10 × 109/L), elevated serum lactate level at the end of surgery, followed by the type of surgery such as coronary artery bypass graft, aortic dissection repair, open heart surgery, and, most importantly, liver transplantation surgery [5,11–15]. In particular, the extravascular lung water index and pulmonary vascular permeability index measured at the end of surgery have been validated as independent predictors of PMV in patients undergoing liver transplantation [14]. However, in addition to traditional clinical predictor studies [5,11–15], genetic research focusing on candidate gene polymorphism is being widely conducted to develop a disease prediction model in various clinical situations [16–27].
Medford et al. [28] conducted a study on the development of acute respiratory distress syndrome (ARDS) in critical patients and showed the statistical correlation of the ARDS incidence with the genetic polymorphisms of vascular endothelial growth factor (VEGF). The study demonstrated higher incidence of ARDS with VEGF polymorphism to be responsible for the increase in microvascular permeability and worsening of clinical statues of patients with ARDS. Kotsaki et al. [24] had identified the association of the early progression of ventilator-related pneumonia in intubated patients with the proof of less proinflammatory cytokine production followed by lipopolysaccharide stimulation in wild type patients, showing the role of single nucleotide polymorphisms (SNPs) within the promoter region of the tumor necrosis factor (TNF) gene for the susceptibility of the host to infection. Other studies had also identified the novel candidate genes in association with the development of acute lung injury and ARDS phenotypes, although the underlying mechanisms of pathogenesis associated with lung injury are still being answered [16,19,25,26].
The assessment of genetic polymorphisms responsible for a patient’s risk of requiring PMV is a challenging task. The early detection of the specific polymorphic genes associated with PMV in patients undergoing liver transplantation surgery could prove to be a useful tool or future biomarkers in postoperative patient management. Moreover, identifying the genetic polymorphisms in this patient population could aid in implementing a personalized treatment strategy for individual patients, based on individual frailty. Therefore, the aim of this study was to determine the perioperative risk factors that affect PMV occurrence after liver transplantation surgery. We particularly sought to investigate the role of candidate gene polymorphisms as independent predictors of PMV after liver transplantation surgery.
Materials and Methods
Patients
In this prospective observational study, we recruited patients between the ages of 20 years and 65 years who were scheduled to undergo living donor liver transplantation surgery. Study approval was obtained from the Institutional Review Board (no. 4-2014-0989) of Yonsei University Health System (Seoul, Korea). Written informed consent was obtained from 140 adult patients (January 2015–January 2018; ClinicalTrials.gov Identifier: NCT02402634). This clinical research was done following the ethical principles for medical research involving human subjects in accordance with the Helsinki Declaration 2013. Patients undergoing mechanical ventilation before surgery, patients currently or previously diagnosed with respiratory disease, and patients with musculoskeletal disorders that may be accompanied by a decreased breathing ability were excluded. Preoperative neurologic evaluations were performed by neurologists, including evaluation for hepatic encephalopathy.
Anesthesia protocols
Anesthesia was inducted with propofol (1.5 mg/kg), sufentanil (1 μg/kg), and rocuronium (0.6–0.8 mg/kg) for muscle relaxation. After endotracheal intubation, desflurane (6–8%) was administered in a 40–50% oxygen-air mixture and an intravenous infusion of sufentanil (0.01–0.025 μg/kg/min) was used for the maintenance of anesthesia. Muscle relaxation was maintained with a rocuronium infusion rate of 0.3 mg/kg/h, which was adjusted to maintain a post-tetanic count of 1-2. The degree of neuromuscular blockade was monitored with an acceleromyograph using train-of-four stimulation (TOF-Watch® SX; Organon Ltd., Ireland) at the adductor pollicis muscle of the right arm. Hemodynamics were monitored and included direct arterial pressures from the radial and femoral artery, central venous pressure from the femoral and internal jugular vein, and cardiac output and pulmonary artery pressure from a pulmonary artery catheter (Swan-Ganz CCombo CCO/SvO2; Edwards Lifesciences, USA). Depth of anesthesia was monitored with bispectral index (BIS, BIS VISTA™, Aspect Medical System Inc., USA) in all patients, and anesthetic agents were adjusted to maintain BIS levels between 40 and 60. Mechanical ventilation parameters were adjusted to maintain PaCO2 values between 30 and 35 mmHg, tidal volume of 6–8 ml/ideal body weight, respiration rate of 10–14/min, and a positive end-expiratory pressure (PEEP) of 5–7 mmHg. Fluid management was maintained with Plasmalyte (Plasma Solution A Inj., CJ Pharma, Korea). Albumin was replaced, based on the albumin level of the patients. Blood products were transfused based on the findings of the complete blood count, prothrombin time, activated partial thromboplastic time, international normalized ratio, and fibrinogen levels during the perioperative period. Inotropic/vasopressor agents were initiated in the event of hemodynamic instability. Hypothermia was prevented by using low-heat blankets, blown heating systems, heat moisture exchanger, and fluid warming systems for all intravenous fluids and blood products.
Mechanical ventilation weaning and extubation
All patients had been discharged to ICU and were administered mechanical ventilation for hemodynamic monitoring on the day of surgery. Chest radiography and arterial blood gas analysis were conducted at least twice daily to observe the initial changes closely. All recipients were ventilated by using a lung-protective ventilation strategy, which consisted of PEEP and low tidal volume (i.e., 6–8 ml/ideal body weight) with permissive hypercapnia. If a patient was hemodynamically stable and oxygenation had improved adequately (i.e., SpO2 > 90%, FiO2 ≤ 0.5, and PEEP ≤ 5 cmH2O), then mechanical ventilator weaning was attempted as soon as possible. All recipients underwent the 1-hour t-tube challenge test to assess the possibility of weaning success and to predict potential complications associated with spontaneous breathing trials. Mechanical ventilation weaning and extubation for every patient were administered by the same intensive care team. The duration of mechanical ventilation after surgery was examined along with the length of ICU and hospital stay, 30-day mortality, and of which PMV was defined as mechanical ventilation for >48 h.
Single nucleotide polymorphism selection and sample collection
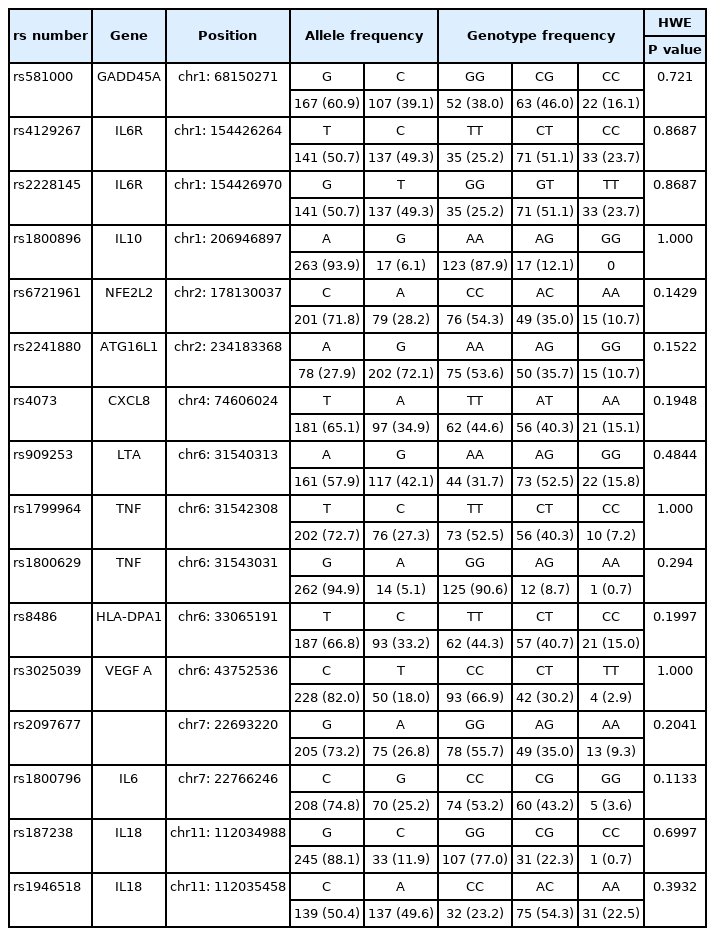
Thirteen established candidate SNPs from 11 genes were selected, based on literature reviews on the genetic involvement in inflammatory-related pulmonary disease. They included rs581000 in the growth arrest and DNA damage inducible alpha (GADD45A) gene; rs18000896 of the interleukin-10 (IL10) gene; rs6721961 of the nuclear factor erythroid 2-related factor 2 (NFE2L2) gene; rs2241880 of the autophagy related 16 like 1 (ATG16L1) gene; rs4073 of the CXC motif chemokine ligand (CXCL8) gene; rs909253 of the lymphotoxin alpha (LTA) gene; rs1799964 and rs1800629 of the TNF gene; rs8486 of the major histocompatibility complex, class II alpha 1 (HLA-DPA1) gene; rs3025039 of the VEGF A gene; rs1800796 of the interleukin-6 (IL6) gene; and rs187238 and rs1946518 of the interleukin-18 (IL18) gene [16-27].
Approximately 2 ml of fasting blood was collected after anesthetic induction prior to surgery from each participant and stored at -80℃. Genomic DNA was prepared from blood samples by using the QuickGene Whole DNA Blood Kit S (Kurabo, Japan), based on the manufacturer’s instructions. All SNPs were genotyped with a single base primer extension assay by using ABI PRISM SNaPShot Multiplex kit (Applied Biosystems, USA), based on the instructions.
Statistical analysis
Statistical analyses were conducted using SPSS version 25.0 (IBM Corp., USA) and SAS software, version 9.1.3 (SAS Institute, Inc., USA). Testing for Hardy–Weinberg equilibrium and allelic association analyses were conducted using the Chi-square test or Fisher’s exact test. The association analyses of PMV with perioperative clinical factors and SNPs are presented with ORs and 95% CIs, using logistic regression models with Bonferroni correction, as appropriate. A value of P < 0.05 was statistically significant.
Results
Baseline characteristics
The baseline characteristics of 140 recipients are summarized in Table 1. Twenty-six (19%) recipients continued to receive mechanical ventilation at 48 h after surgery, while 114 recipients were weaned from mechanical ventilation within 48 h after surgery. The mean age of the PMV group and non-PMV group was 53.5 ± 11.7 and 55.7 ± 8.4 yr, respectively. Statistically significant between-group differences existed in sex distribution (the female-to-male ratio of the PMV group and non-PMV group were 1.36 and 0.36, respectively with P = 0.002). The preoperative model for end-stage liver disease (MELD) score, presence of underlying diabetes, coagulopathy, intraoperative continuous renal replacement therapy (CRRT), and smoking status were also significantly different between the two groups: the MELD score, prevalence of coagulopathy, and use of intraoperative CRRT were higher in the PMV group, and the prevalence of underlying diabetes and smoking history was higher in the non-PMV group. Detailed differences of other perioperative parameters between the two groups were shown in Supplementary Table 1. However, no significant difference was observed with respect to the presence of congestive heart failure, chronic obstructive pulmonary disease, preoperative respiratory complications, and the duration of surgery.
SNP genotypes with PMV
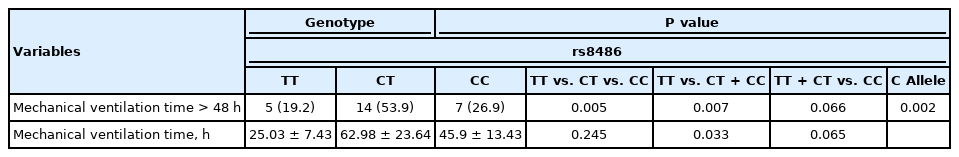
Genotype frequency of all candidate SNPs were in Hardy–Weinberg equilibrium (P > 0.05) (Table 2). Significant differences in the genotype frequency of rs1800629 and rs8486 were noted between the PMV and non-PMV groups: the PMV group had a higher frequency of A and C alleles (P = 0.025 and P = 0.002, respectively) and a lower frequency of GG and TT genotypes in the rs1800629 and rs8486 polymorphisms (P = 0.045 and P = 0.004, respectively) (Supplementary Table 2).
Dominant, recessive, codominant, and allele models were adopted to evaluate the associations of the candidate gene polymorphisms with PMV, patient demographics, and perioperative data (Table 3). The stepwise logistic regression analysis revealed that a mutation at rs8486 in the HLA-DPA1 gene (OR: 8.060, 95% CI [1.451, 44.765], P = 0.017), the use of intraoperative CRRT (OR: 24.731, 95% CI [1.077, 567.915], P = 0.045), and the level of serum lactate in postoperative 24 h (OR: 3.008, 95% CI [1.497, 6.045], P = 0.002) were significantly associated with a higher risk for PMV (Table 4).
Discussion
We examined the association between candidate gene polymorphisms, related perioperative clinical factors, and the risk of PMV in liver transplantation recipients. Our results suggested that the application of intraoperative CRRT, an elevated serum lactate level during the postoperative period, and the minor allele of the rs8486 gene polymorphism in HLA-DPA1 were risk factors for the development of PMV in liver transplantation recipients.
Previous studies [15,29] have also highlighted the high incidences and the deleterious clinical outcomes of postoperative pulmonary complications after liver transplantation surgery. Various definitions of PMV during the postoperative period have been proposed [6-10]; therefore, our study defined PMV as the requirement for mechanical ventilation for > 48 h postsurgery. Among our patients, 18.6% of patients were in this category. Recently published studies [30,31] investigating the incidence of PMV among liver transplantation patients report that from 10% to 50% of patients underwent PMV or remained intubated, whereas other patients were immediately extubated at the end of surgery. However, the discrepancy in the percentage of patients undergoing PMV may be related to different patient demographics; hospital size; the workmanship of the transplant and critical care team; and the difference in each hospital’s enhanced recovery after surgery protocols, including early endotracheal extubation in the operating room.
Many studies have focused on the stratification of risk factors for PMV [5,11–15]; however, applying a unified standard to different hospitals and patients’ settings is difficult because each hospital and clinical doctor has different protocols and clinical guidelines for different patient groups and hospital situations. Therefore, finding more robust risk factors that are not largely affected by the surroundings such as genetic data is important.
Numerous studies have shown that the susceptibility of respiratory-related diseases is affected by polymorphisms in many genes, including GADD45A, IL-10, NFE2L2, TNF-α, VEGF A, IL-6, IL-18, and HLA-DPA1 [16,18,19,23–27]. The HLA region, located on chromosome 6, is characterized by high gene density, variability, and extensive linkage disequilibrium. The HLA region encodes hundreds of genes with an immunological function and proteins with critical roles in immunity such as antigen processing and presentation, and self-recognition by immune cells such as ligand receptors, cytokines, signaling factors, heat shock proteins, and transcription regulators. The HLA region is also involved in many biological processes such as histocompatibility, inflammation, ligands for immune cell receptors, and the complement cascade [32,33]. The role of HLA as an immune-inhibitory molecule has been investigated in the field of inflammatory conditions; neoplasms such as hematolymphoid neoplasms, visceral carcinomas, dermal-based neoplasms; and, recently, in the pathogenesis of respiratory syndrome outbreaks in coronavirus disease 2019 [34] for which a strong association has been demonstrated between HLA ligands and increased susceptibility to respiratory infection. In addition, the SNP rs8486 polymorphism has a functional consequence such as the 3′-UTR variant; therefore, genetic variation in the 3′-UTR variant can also affect gene expression that interferes with micro-RNA binding [35]. The result of minor allele of rs8486 gene polymorphism to be the risk factor for the development of PMV in liver transplantation recipients is in collusion with the likelihood of minor alleles to become risk alleles in the published genome wide association study on complex diseases [36]. However, functionality of such changes requires empirical confirmation in further studies.
Our study successfully demonstrated a significant relationship of rs8486 SNP encoding HLA-DPA1 with PMV and with the duration of mechanical ventilation after liver transplantation surgery. The candidate gene search was conducted using a published gene database and with a focus on respiratory-related infection and innate inflammatory-related genes. However, our patients’ data only showed a significant relationship with the sole HLA-DPA1 gene, along with clinical factors such as an elevated postoperative serum lactate level and intraoperative CRRT. SNP rs1800629, which encodes the traditional inflammatory cytokine TNF-α had a significant relationship before multivariate regression; however, it ultimately failed to show a correlation, along with clinical factors. A race-specific gene database search was conducted with the necessary statistical confirmation; however, the small number of patients may have limited the achievement of statistical significance in this study.
In addition to genetic factors, an elevated serum lactate level and the application of intraoperative CRRT had a significant effect on the occurrence of PMV. Serum lactate levels have especially been emphasized as a good predictor for delayed endotracheal extubation among liver transplantation recipients [37]. It has also been highlighted as a significant risk factor for increasing the postoperative risk of morbidity and mortality [38] and prolonging the length of hospital stay [39]. These findings are consistent with the findings of this study. Hyperlactatemia could be caused by the higher production and lower clearance of lactate because of a pathologic process such as decreased renal function and could result in the application of CRRT. The origin of hyperlactatemia after liver transplantation surgery can be multifactorial and includes primary nonfunction of the newly grafted liver, substantial surgical blood loss with hypoperfusion, high-dose vasopressor use, acute kidney injury and oliguria, and organ ischemia and reperfusion during surgical procedures [40,41]. Organ ischemia induced by lower perfusion and lower oxygen utilization during the anhepatic phase are associated with an elevated level of lactate into the systemic circulation because of decreased washout and subsequent metabolic acidosis during reperfusion. Such an imbalance of oxygen supply and organ consumption results in a poor patient outcome, including PMV. A previously published study has confirmed that longer ventilation time and the need for reintubation and tracheostomy were associated with postoperative hyperlactatemia after major surgery [39].
CRRT can be applied to patients with refractory renal dysfunction to manage uncontrolled metabolic acidosis, electrolyte imbalance, volume overload, and brain edema, accompanied by hemodynamic instability. Many institutions apply intraoperative CRRT for liver transplantation recipients with severe preoperative renal dysfunction to prevent critical uremic challenges and to facilitate fluid management during surgery. Its application is regarded as a successful management method during liver transplantation surgery [42,43]. Despite the clinical advantages of CRRT, underlying hemodynamic instability and decreased renal function of patients receiving CRRT make applying intraoperative CRRT as the prominent risk factor for morbidity, mortality, and other poor outcomes such as PMV in patients undergoing liver transplantation surgery. Previously published studies have likewise reported a greater number of patients who received CRRT in the PMV group posttransplant [15], and a higher risk of respiratory failure requiring intubation among critically ill patients who needed CRRT [44]. However, other renal-related factors such as the duration of CRRT, severity of underlying renal dysfunction, and modality of renal replacement therapy also have a role in postoperative mechanical ventilator care or intensive care; therefore, further in-depth analysis and study are required to clearly demonstrate the effect of CRRT on PMV.
A high MELD score and coagulopathy are also well-known risk factors for posttransplantation and postsurgery morbidity and mortality [45,46]. Such risk factors could contribute to the decreased diffusion capacities and could possibly affect the onset of respiratory complications and PMV among transplantation recipients [46,47]. With regard to coagulopathy, excessive fluid administration and positive fluid balance significantly lower respiratory compliance, which is highly suggestive of the occurrence of post-liver transplantation acute lung injury and severe ARDS caused by volume overload, massive blood transfusion, severe ischemia–reperfusion syndrome, and systemic infection [48].
A history of diabetes has an inconsistent effect on PMV. Such various results with less statistically significant finding are probably because of diverse confounding factors of diabetes such as the type and duration of diabetes, glycosylated hemoglobin (HbA1c) levels, type of medications, and the use of insulin. Patients diagnosed with diabetes in our group had a median (Q1, Q3) duration of diabetes of 7 (2, 10) years. Each patient had regularly taken antidiabetic medication with an average HbA1c level of 6.5 ± 1.4%. Such differences in the patient population could have resulted in the discrepancy toward PMV and respiratory complications reported in other previously published studies [21,49]. The same explanation could be adopted for smoking history in that nonsmoking patients were more often in the PMV group.
The current study had several limitations. First, the small sample size and the homogeneity of the study group limit in-depth subgroup analysis and applying the results universally to different ethnic groups. However, various genetic studies are actively being conducted that especially target Caucasians. Therefore, we believe that genetic information focusing on Asian populations is also significant in the field of patient management. Moreover, further studies with a larger sample size are needed to verify the findings, along with in-depth statistical approach to show the diagnostic probabilities.
Second, novel technologies are being rapidly introduced in the field of genetic studies; therefore, more affluent genomic information could have been obtained by means of genome-wide studies using genotyping arrays or exome whole genome sequencing. However, these latest technologies have the limitations of high costs and statistical burden.
This study identified the rs8486 polymorphism in HLA-DPA1 as a gene associated with PMV in liver transplantation recipients, as were intraoperative CRRT application, and an elevated lactate level during the postoperative period.
Acknowledgements
The authors thank the Medical Research Support Services of Yonsei University College of Medicine (Seoul, South Korea) for the statistical support related to this work.
Notes
Funding
This study was supported by the Faculty Research Grant from Yonsei University College of Medicine (Grant no. 6-2015-0020).
Conflicts of Interest
No potential conflict of interest relevant to this article was reported.
Author Contributions
Eun Jung Kim (Conceptualization; Data curation; Formal analysis; Investigation; Methodology; Resources; Software; Validation; Visualization; Writing – original draft; Writing – review & editing)
Min-soo Kim (Conceptualization; Data curation; Formal analysis; Methodology; Supervision; Validation; Writing – review & editing)
Myoung Soo Kim (Data curation; Supervision; Writing – review & editing)
Junhyun Nam (Data curation; Methodology; Writing – review & editing)
Seung Ho Choi (Conceptualization; Data curation; Funding acquisition; Investigation; Methodology; Project administration; Resources; Supervision; Validation; Writing – review & editing)
Supplementary Materials
Perioperative findings of the liver transplantation recipients
Single nucleotide polymorphism genotypes in the PMV and non-PMV groups