Introduction
For more than a decade, anesthesia has been traditionally administered by conventional mask anesthesia using the Goldmann dental mask and endotracheal intubation (ETI) [
1]. Since Dr. Archie Brain introduced the laryngeal mask airway (LMA) in 1981, supraglottic airway devices (SADs) have begun to replace ETI for resuscitation and difficult intubation as well as for general anesthesia [
2,
3]. SADs are able to maintain stable hemodynamics while requiring less anesthesia than ETI [
3].
Over the years, many newer devices have evolved for clinical use, including the i-gel, LMA Supreme, and Ambu AuraGain. Among these second-generation devices, the i-gel airway (Intersurgical Ltd., UK) has a soft, flexible, gel-like texture and is made of a thermoplastic elastomer non-inflatable cuff to create a seal with the peri-laryngeal structures [
1,
4ŌĆō
6].
The LMA Supreme (Teleflex Medical, Co., Ireland), which has many similarities to the i-gel, is another disposable second-generation SAD that is made of silicone with an inflatable cuff and a curved, anatomically shaped semi-rigid airway tube that is elliptical in cross section [
7,
8].
The Ambu AuraGain (Ambu A/S, Denmark) is a newer, second-generation SAD that was launched in June 2014 [
1]. It is also a disposable device made of polyvinyl chloride and has a preformed curve that follows the human airway [
9ŌĆō
11].
These recently-introduced second-generation SADs have a gastric channel to minimize the risk of aspiration resulting from gastric insufflation. Hence, they can be used in elective laparoscopic surgeries as well as for difficult intubations and resuscitations. Although these devices have been extensively studied individually, no study has compared all three devices collectively in elective surgeries. Therefore, we designed this study to evaluate the clinical performance of the i-gel, LMA Supreme, and Ambu AuraGain in adult non-obese patients under general anesthesia. The primary objective of our study was to determine and compare the insertion times of these three SADs. The ease of insertion, number of insertion attempts, oropharyngeal leak pressure (OLP), airway maneuver requirement, gastric tube placement difficulty, and any other complications were also assessed.
Materials and Methods
This study was approved by the Institutional Review Board (97th ECM II B/P28). A total of 90 male and female patients aged 18ŌĆō65 years with an American Society of Anesthesiologists (ASA) physical status IŌĆōIII undergoing elective surgery lasting < 2 h under general anesthesia at the Department of Anesthesiology, King George Medical University, Lucknow (Ref. no. ECR/262/Inst/UP/2013/RR-16) were included. The study was also registered under the Clinical Trial Registry of India (Registration no. CTRI/2020/01/022633). Informed and written consent was obtained from all study participants. This study was conducted in accordance with the ethical principles of the Helsinki Declaration-2013 and followed good clinical practice guidelines.
Patients with any of the following were excluded from the study: risk of aspiration, body mass index (BMI) > 35 kg/m2, unstable vital signs, anticipated difficult airway, high possibility of respiratory complications (asthma, chronic obstructive pulmonary disease, or recent pneumonia), history of obstructive sleep apnea, and history of gastroesophageal reflux disease.
Thirty subjects each were randomly allocated to the i-gel (I), LMA Supreme (L), or Ambu AuraGain (A) group using computer-generated software
Based on the ASA guidelines, all patients fasted for at least 8 h before the surgery and were premedicated with oral alprazolam 0.25 mg and ranitidine (150 mg) on the night before surgery.
Upon arrival to the operating room, noninvasive blood pressure, pulse oximetry (SpO2), electrocardiogram, and end-tidal carbon dioxide monitoring were initiated according to the ASA standards. All patients received intravenous (IV) ondansetron 0.1 mg/kg and IV midazolam 0.01 mg/kg. Preoxygenation was performed for 3 min with 100% O2 at 8 L/min of fresh gas flow (FGF). Anesthesia was induced by IV fentanyl (2 ╬╝g/kg) and IV propofol 1.5 mg/kg. After the eyelash reflex disappeared, the subjects were paralyzed with a loading dose of IV vecuronium (0.1 mg/kg).
Mask ventilation of the lungs was performed through a facemask with O2 at 6 L/min of FGF for 3 min. After lubricating with water-soluble gel and determining the size of the device (depending on the patientŌĆÖs weight and according to the manufacturerŌĆÖs instructions), the device was inserted in accordance with the manufacturersŌĆÖ recommendations by one of the three study investigators, each of which had previously inserted more than 400 SADs in clinical practice, with a minimum of 30 prior insertions for each device. After device insertion, the cuff was inflated and the intra-cuff pressure was then standardized to 60 cmH2O (based on the manufacturersŌĆÖ recommendations) in Groups L and A. An appropriately sized RyleŌĆÖs tube was then inserted through the gastric port of the device. A visible chest rise and end-tidal carbon dioxide waveform with gentle squeezing of the bag was used to confirm the appropriate placement of the SAD.
Patients were then connected to the anesthesia delivery system and mechanical ventilation was initiated with the tidal volume set at 8 ml/kg and the respiratory rate between 14 and 18 breaths/min. An FGF mixture of 3 L/min (oxygen 2 L/min and nitrous oxide 1 L/min) was maintained on 2% sevoflurane and IV vecuronium (0.01 mg/kg to maintain end-tidal carbon dioxide between 35 and 40 mmHg). An unblinded observer who was not part of the study performed the data collection.
The device insertion time was calculated from the time of picking the device till the appearance of the square wave end- tidal carbon dioxide upstroke. Other outcomes measured included the OLP, the ease of insertion, first attempt rate, overall success rate, airway maneuver requirement for successful ventilation, and any associated postoperative complications.
The OLP was determined by an audible leak over the patientŌĆÖs mouth upon closing the expiratory valve at 30 cmH2O with a gas flow of 3 L/min. If there was no audible leak, a stethoscope was placed over the trachea to listen for the leak. The OLP was measured 15 min after device insertion.
The ease of insertion was evaluated according to the resistance to insertion of the SAD on a four-point rank scale between 1 and 4 (1 = no resistance, 2 = mild resistance, 3 = moderate resistance, 4 = unable to pass the device). The number of attempts was also recorded. Device insertion was considered successful if the device was inserted in the first or second attempt after any airway maneuvers. The attempt was considered a failure if more than two attempts were needed and if the airway was secured using a tracheal tube. Maneuvers for successful ventilation included inserting the device further, head extension, and jaw thrust. An inadequate oxygenation/ventilation situation (inability to generate 6ŌĆō8 ml/kg tidal volume during positive pressure ventilation, a rise in end tidal carbon dioxide > 50 mmHg despite airway maneuvers or device adjustments, or an SpO2 < 90%) during surgery was also considered a device failure, and ETI was performed.
After the surgical procedure, sevoflurane was discontinued and IV neostigmine (50 ╬╝g/kg) and glycopyrrolate (10 ╬╝g/kg) were administered to antagonize the residual neuromuscular block. The SAD was removed when the patient was fully awake and checked for any complications, including coughing, bronchospasm, desaturation, blood staining, and the presence of tongue, teeth, or lip injury. All patients were observed for 1 h postoperatively. Any sore throat, dysphagia, dysphonia, or numbness of the lip was evaluated immediately in the postoperative care unit after surgery.
Statistical analysis
All statistical analyses were performed using SPSS (IBM, SPSS Inc., USA) version 21.1 statistical analysis software. Continuous data were analyzed using the StudentŌĆÖs t-test. For categorical data, the chi-square test was used. Since there were three groups, ANOVA was used for the analysis. For all analyses, statistical significance was set at P < 0.05. The sample size was calculated using the time of insertion as the primary objective (to detect a difference of 4 s), with a standard deviation of 4.2 [
12], a power of 0.9, and an alpha value of 0.05 (two-sided). The results indicated that each group needed a minimum of 26 subjects. Taking into consideration a dropout rate of 10%, 30 patients were enrolled in each group.
Results
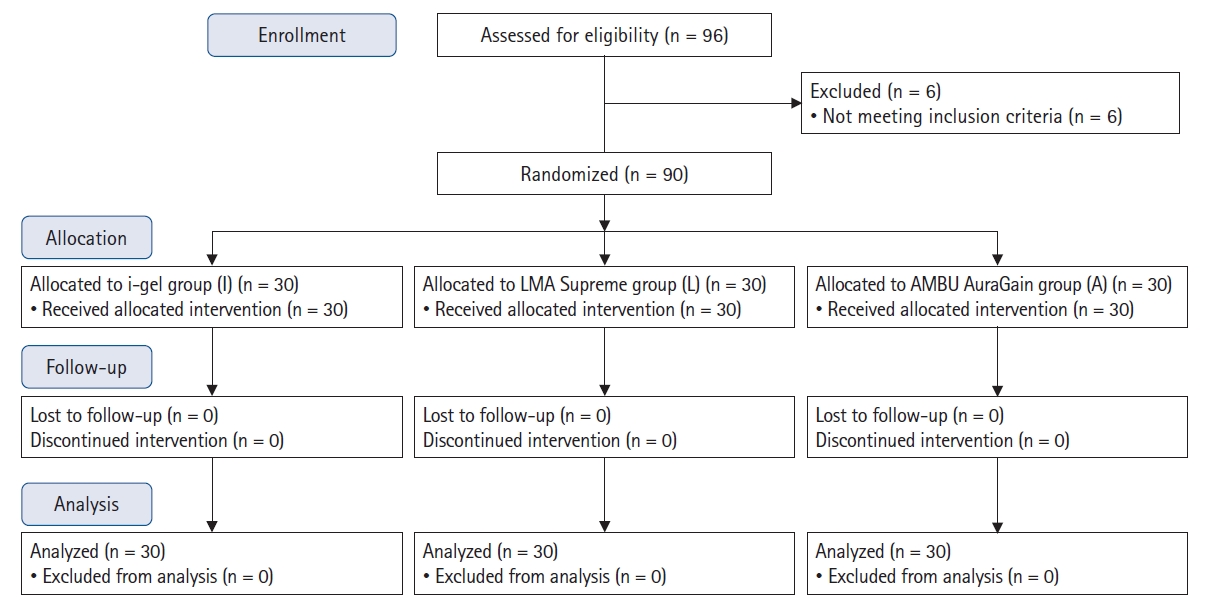
Ninety-six patients were assessed for eligibility, six of which were excluded (two had high blood pressures and four had loose teeth). Thus, 90 patients were randomly allocated into Groups I, L, and A (
Fig. 1).
In this study, the demographic variables of age, sex, body weight, height, BMI, Mallampati score, and ASA physical status classification were comparable among the groups, with no statistically significant differences (P > 0.05), as shown in
Table 1.
Various aspects related to device insertion, such as the size, number of attempts, insertion time, OLP, ease of insertion, device failure, airway maneuver requirements, and difficulty with gastric tube placement, are listed in
Table 2. Group I (16.9 ┬▒ 4.9 s) had a significantly shorter insertion time than Group L (19.6 ┬▒ 5.2 s) and Group A (22.1 ┬▒ 5.7 s) (P = 0.001). The OLP at 15 min for Group A (29.8 ┬▒ 3.0 cmH
2O) was higher than that for Group L (24.1 ┬▒ 6.3 cmH
2O) and Group I (9.4 ┬▒ 6.1 cmH
2O) (P < 0.001).
The adverse events and complications among the three groups were comparable and not statistically significantly different, as shown in
Table 3.
Discussion
In this study, we compared the clinical performance of three SADs in non-obese patients under general anesthesia. While previous studies have evaluated these devices individually or compared two of them, there is a paucity of studies that have compared all three of these devices in a single study.
In our study, we found that the i-gel, LMA Supreme, and Ambu AuraGain are effective and convenient in non-obese patients under general anesthesia. Insertion time, which is an important determinant during emergencies and for resuscitation, was considered the primary objective in this study. Longer insertion times may cause more interruption during chest compressions and increase the chances of neurological and respiratory morbidity during resuscitation attempts. In addition, increased apnea time may lead to an increase in blood CO
2 levels and may jeopardize the acid-base balance. Avoiding any possible delay in airway management is an important aspect to consider for the clinical research of SADs. Among the three SADs, the i-gel had the shortest insertion time. This device has previously been shown to have a comparably shorter insertion time, both in a study of adult patients undergoing laparoscopic cholecystectomy by Sabuncu et al. [
12] and in a study of geriatric patients by In et al. [
3]. This could be explained by the absence of an inflatable cuff, since additional time is required to inflate the cuff to provide optimal cuff pressure for both the LMA Supreme and Ambu AuraGain devices. To limit the bias associated with device familiarity in this study, only clinicians who had successfully inserted each of the SADs a minimum of 30 times before the study were permitted to perform the device insertions.
Similar to our study, Wong et al. [
10] found that the insertion time was longer for the Ambu AuraGain than for the LMA Supreme. In our study, a mean difference of 2.5 s in insertion time was found between the LMA Supreme (19.6 s) and Ambu AuraGain (22.1 s). In another study, Shariffuddin et al. [
13] found that the Ambu AuraGain took a mean 6 s longer to obtain the first capnograph trace compared to the LMA Supreme. The authors of that study attributed this to the structural differences between the two devices, since the Ambu AuraGain has a less pliable firm tip and bulky posterior curvature with a larger cuff to provide better sealing pressures [
13], while the LMA Supreme has a hard tube wall pre-shaped according to the anatomical curve, and the radian design makes the front end of the ventilation tube and the laryngeal vestibule form an effective orientation, enabling quicker insertion [
14].
Regarding ease of insertion, no resistance was observed in 80% (72/90) of our study population, and close to 90% (80/90) of the patients in our study had successful insertions in the first attempt. The first-attempt success rate was found to be comparable among the groups. Our results are consistent with those of Teoh et al. [
15], who found that 47 (94%) LMA Supremes and 48 (96%) i-gels were successfully inserted on the first attempt. This could be due to the lower Mallampati scores (I, II) and normal airways in our patient population (83/90) and the cliniciansŌĆÖ considerable experience.
We had no device insertion failures, in contrast to the seven observed by Shariffuddin et al. [
13], and we had a high first-pass success rate among all three groups. Both of these differences can be explained by the use of neuromuscular blocking agents in our study, which may have provided better muscle relaxation and thereby facilitated easier insertion. Regarding the airway maneuver parameter, the majority of cases (93.3%) did not require any airway maneuvers; however, six cases (6.7%) required airway maneuvers for the device to be inserted further. The Ambu AuraGain required more airway maneuvers than the i-gel or the LMA Supreme.
In our study, the Ambu AuraGain achieved the highest OLP among the three SADs, followed by the LMA Supreme and the i-gel. OLP is a significant characteristic feature that determines the efficiency of a supraglottic device. It defines the sealing capability between the device and supraglottic mucosa. The better sealing pressures observed in Group A in our study reconfirm previous findings by Lopez et al. [
7] and Wong et al. [
10]. The wider airway tube and prominent posterior cuff design of the Ambu AuraGain provides a tighter and more consistent perilaryngeal seal, as explained in previous studies [
7]. The higher OLP with the Ambu AuraGain makes it more suitable for positive pressure ventilation along with reduced aspiration risks.
Despite the low OLP in the i-gel group in our study, none of our study patients experienced inadequate oxygenation/ventilation. This could be explained by the better chest compliance in our patient population (since we excluded patients with obesity, restrictive lung disease, and any pulmonary pathology) and the structure of the i-gel device, which is fabricated with a thermoplastic elastomer (styrene ethylene butadine styrene) to provide improved sealing pressures when its warmed up to body temperature. The low OLP observed in the i-gel study group could also have been a consequence of the fact that we had to reuse some i-gel devices after sterilization because of the unavailability of the device due to the COVID-19 pandemic lockdown in our setup. Two size 4 i-gels were reused for six patients in our study. Before reuse, we ensured that no device was visibly physically damaged. Previous studies [
16,
17] have confirmed that there is no difference in leak volumes and leak fraction (defined as the leak volume divided by the inspired tidal volume) between the i-gel and endotracheal tubes in non-obese patients.
Difficulties with gastric drain insertion was comparable among the groups, although it was most difficult with the i-gel device. Teoh et al. [
15] suggested that the likely reason for this difficulty is the smaller size of the aperture for the gastric access port with the i-gel. In a study conducted by Joshi et al. [
18], gastric drain insertion was reported to be easier with the Ambu AuraGain due to the reduced friction in the inner surface of its polyvinyl material and its short and wide gastric channel [
11]. Fernandes et al. [
19] also reported that the placement of gastric tubes in the i-gel was more difficult due to the narrow tract of the i-gel.
The postoperative complications among the groups were comparable, with no statistically significant difference among them. Nausea was seen in 11% (10/90) and sore throat was present in 12% (11/90) of the patient population. In previous studies, the incidence of postoperative sore throat varied from 3ŌĆō10% for the Ambu AuraGain and 0ŌĆō38% for the LMA Supreme [
7,
13]. The incidence of sore throat was lower in our study, which can be explained by our better lubrication and shorter duration of surgery (< 2 h). There was no nerve damage or trauma to any of the perilaryngeal structures of the oral cavity. Blood staining occurred in only one patient. LŌĆÖHermite et al. [
20] compared the incidence of sore throat following the insertion of three SADs (LMA Unique, LMA Supreme, and i-gel) and reported that the incidence of sore throat was similar among the three devices.
Despite the effective measures taken, this study had some limitations. First, our study only included subjects who were not obese and had normal BMIs, and blinding was not possible. Additionally, hemodynamic monitoring was not performed, though it could have improved the study. Fiberoptic bronchoscopy was not used to assess the anatomical position of the seal, as it was logistically not feasible to perform bronchoscopy in all cases. Finally, we reused the i-gel devices for six of our patients, which could have affected our results.
In conclusion, our study demonstrated that all three devices are convenient and effective for airway management in non-obese adults under general anesthesia. However, the shorter insertion time required for the i-gel may make it more suitable for resuscitation and emergencies, while the maximum OLP associated with the Ambu AuraGain may make it more useful for reducing aspiration risk.