Designing the ideal perioperative pain management plan starts with multimodal analgesia
Article information
Abstract
Multimodal analgesia is defined as the use of more than one pharmacological class of analgesic medication targeting different receptors along the pain pathway with the goal of improving analgesia while reducing individual class-related side effects. Evidence today supports the routine use of multimodal analgesia in the perioperative period to eliminate the over-reliance on opioids for pain control and to reduce opioid-related adverse events. A multimodal analgesic protocol should be surgery-specific, functioning more like a checklist than a recipe, with options to tailor to the individual patient. Elements of this protocol may include opioids, non-opioid systemic analgesics like acetaminophen, non-steroidal anti-inflammatory drugs, gabapentinoids, ketamine, and local anesthetics administered by infiltration, regional block, or the intravenous route. While implementation of multimodal analgesic protocols perioperatively is recommended as an intervention to decrease the prevalence of long-term opioid use following surgery, the concurrent crisis of drug shortages presents an additional challenge. Anesthesiologists and acute pain medicine specialists will need to advocate locally and nationally to ensure a steady supply of analgesic medications and in-class alternatives for their patients’ perioperative pain management.
Introduction
Worldwide, today’s healthcare environment stresses the provision of high-quality care while reducing costs. In the United States (US), federal payments to healthcare providers have been tied to various activities: participation in improvement projects, quality metrics, and resource utilization through pay-for-performance programs such as the Merit-Based Incentive Payment System (MIPS) developed by the Center for Medicare and Medicaid Services (CMS) [1]. This growing trend is taking place in other industrialized countries that face the dilemma of rapidly rising healthcare costs [2] and is, in part, responsible for recent innovations in hospital-based care. In the perioperative setting, implementation of standardized multimodal analgesia (MMA) represents one such innovation.
MMA can be defined as the use of more than one pharmacological class of analgesic medication targeting different receptors along the pain pathway with the goal of improving analgesia while reducing individual class-related side effects [3]. The concept of MMA is not new, but the current need for MMA and minimizing opioid use is clearly evident in light of the opioid epidemic as well as ubiquitous drug shortages facing the US and other countries. MMA is recommended for postoperative pain in many clinical situations and is the key focus of a joint clinical practice guideline from the American Pain Society, American Society of Regional Anesthesia and Pain Medicine (ASRA), and the American Society of Anesthesiologists [4]. Designing an ideal perioperative pain management strategy should always start with MMA, and this article will review the evidence for this recommendation including support for individual components and the role of MMA in addressing the opioid epidemic. In this review, we will examine MMA both in the broader context of perioperative care as well as in its specific application in patients undergoing total knee arthroplasty (TKA), a procedure that has been the focus of substantial attention as some projections predict 3.48 million primary and 268,200 revision TKA procedures will be performed annually by 2030 [5].
Elements of Multimodal Analgesia
Perioperative pain consists of multiple pain subtypes and as such cannot be effectively treated with a single medication. Surgical pain may be nociceptive, neuropathic, mixed, psychogenic, or idiopathic [6], depending on the surgery. Kehlet and Dahl [7] recognized the value of balanced analgesia or MMA over two decades ago when they published one of the earliest papers advocating the use of multiple agents rather than a single agent in treating postoperative pain. A good MMA protocol is a checklist rather than a recipe; it will standardize the categories of analgesics while still allowing for some flexibility in the individual components based on patient comorbidities, allergies, medications, and previous surgical experiences. For example, although gabapentinoids have been shown to be opioid sparing when part of a multimodal protocol [8], they can cause sedation [9], particularly in the elderly, and a protocol that includes gabapentinoids may have limitations on the maximum patient age for the drugs or a dose adjustment. A patient with a sulfa allergy may present for elective TKA which precludes celecoxib; rather than eliminating all cyclooxygenase (COX) inhibitors, an alternative, such as ibuprofen or naproxen, can be given. Anticipating common allergies and side effects in certain populations will help maintain adherence to multimodal protocols.
Non-opioid systemic analgesics
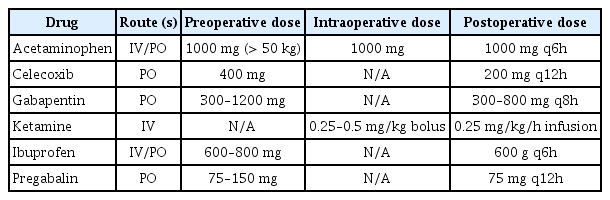
Non-opioid analgesics are the cornerstone on which to build a successful perioperative MMA regimen (Table 1). In addition to the absence of opioid side effects, many of these agents are highly effective in reducing postoperative pain and allowing for faster mobilization and meeting milestones. The first medication, acetaminophen, is one that has been in clinical use for decades with a proven track record of safety when used in appropriate doses. Many current multimodal protocols include acetaminophen [8,10,11], and its opioid-sparing effects and absence of contraindications outside of severe liver disease make it appealing. Though not adequate alone for painful procedures such as TKA, it is definitely a useful and inexpensive component of the protocol. Current evidence does not support the use of intravenous (IV) acetaminophen over oral (PO) acetaminophen universally [12], but for specific indications (e.g., long procedures or patients not able to take PO medications) the IV formulation is a good option.
Non-steroidal anti-inflammatory drugs (NSAIDs) represent another class of medication that is highly effective for perioperative pain management and should be considered for MMA protocols. NSAIDs exert their effects through inhibition of COX and prostaglandin synthesis [8]. Despite concerns about the increased risk of postoperative bleeding with NSAIDs, a meta-analysis has revealed that ketorolac does not increase the risk of perioperative bleeding [13]. In a systematic review, the combination of ibuprofen 400 mg and paracetamol (i.e., acetaminophen) 1000 mg had a number needed to treat of only 1.5 to achieve 50% postoperative pain relief or greater [14]. Caution should be exercised in patients with renal disease and gastrointestinal ulcers [8]. In addition, all NSAIDs increase the risk of cardiovascular events, including myocardial infarction [15]. In patients in whom gastrointestinal ulcers are of particular concern, a COX-2 selective inhibitor may be substituted for a non-selective agent to decrease this risk [16].
Another class of analgesics commonly used in MMA protocols is the gabapentinoids, which include gabapentin and pregabalin. As anti-convulsants they exert their clinical effects via interaction with voltage-gated calcium channels [17]. Meta-analyses have demonstrated that gabapentin [18] and pregabalin [19] improve postoperative pain when part of a MMA regimen but are associated with sedation. In particular, elderly patients are vulnerable to this side effect, and consideration should be given to lowering the dose or avoiding them altogether. For patients who may have symptoms that suggest neuropathic pain, such as pain with a burning quality, these agents may be particularly useful.
Other agents to consider in MMA protocols include N-methyl-D-aspartate (NMDA) antagonists, with focus on ketamine and magnesium in particular. Ketamine has a clear opioid-sparing effect in the perioperative period [20] and may even reduce long-term opioid consumption in opioid-tolerant patients [21] as well as persistent postsurgical pain when used intravenously [22]. It is increasingly being featured in MMA protocols as an opioid alternative [23]. Although reviews have not consistently shown an increased incidence of side effects compared to controls [20,24], ketamine has the potential to cause psychomimetic effects and this should be factored into treatment decisions. Its benefits are maximized during painful surgery, including TKA, and opioid-tolerant patients may particularly benefit. ASRA has recently published guidelines for the use of ketamine in acute pain management [25].
Magnesium has produced mixed results as a postoperative analgesic when used alone [26,27] but has demonstrated synergism when combined with morphine or ketamine [26]. It is thought to exert its effects via spinal NMDA receptors and appears to be more effective when used intrathecally rather than intravenously [26]. Nevertheless, it is an inexpensive addition to a multimodal regimen that may be considered especially if there are contraindications or allergies that limit the use of other non-opioid agents.
Local Anesthetics
Regional anesthesia and analgesia techniques
Any discussion of MMA and opioid-sparing techniques must include regional anesthesia, which is the use of local anesthetics to anesthetize discreet areas of the body. Regional anesthesia provides superior pain control compared to traditional opioid-based strategies in many types of surgery, including TKA [28], shoulder surgery [29], foot and ankle surgery [30], and colorectal surgery [31] and can decrease nausea and vomiting as well as the time spent in the post-anesthesia care unit [32]. Regional anesthesia includes both neuraxial (spinal and epidural) anesthesia and peripheral nerve blocks. For surgical procedures amenable to regional anesthesia, such as upper or lower extremity surgery, incorporating blocks can be a highly effective method of minimizing opioids and providing excellent analgesia. Nerve blocks do carry a risk of complications, including nerve injury, bleeding, infection, and rebound pain, and these should be weighed against the potential benefits. Nerve block duration can be prolonged by either placing a continuous nerve block (i.e., perineural catheter) [33] or adding adjuvants to the perineural mixture. Although not approved for this indication in the US, perineural dexamethasone has been shown to extend the duration of brachial plexus block by 6–8 h [34] and sciatic nerve block by 13 h [35]. Dexmedetomidine can prolong blocks as well, with a mechanism likely similar to clonidine, although bradycardia may be an issue [36].
Continuous peripheral nerve blocks offer an alternative to adjuvants to extend the effects of nerve blocks if trained staff are available and a system is in place to care for the patients who receive them. For TKA, one study concluded that single-injection adductor canal block (ACB) is non-inferior to continuous ACB regarding pain and opioid consumption in 48 h [37]. This is encouraging for those practices that do not have resources in place for continuous nerve block follow-up. Another recent study has concluded that a continuous femoral nerve block may not decrease pain or opioid consumption compared to single-injection femoral nerve block after TKA [38]. That being said, continuous peripheral nerve blocks tend to result in less nausea, fewer opioids, and greater satisfaction with pain management overall than alternative techniques [39]; they also allow for individual titration of effect, prolongation of analgesia when needed, and patient-controlled analgesia. Although the addition of perineural adjuvants like dexamethasone may raise concern for neurotoxicity based on animal studies [40], this has not been consistently borne out in human studies [41]. Therefore, the choice of adjuvant or catheter-based technique should be specific to the practice and may be made based on the training of personnel, experience, and logistics.
Local infiltration analgesia
Some surgeons may prefer the injection of local anesthetics directly into the vicinity of the wound for certain surgeries rather than regional anesthesia for various reasons, including concerns over motor weakness, the need to check nerve function postoperatively, or system-related issues. Wound infiltration techniques have been shown to provide some analgesia for laparoscopic cholecystectomy [42] and cesarean section [43], but the magnitude of analgesia and opioid sparing appears to be small and short-lived. Nevertheless, if peripheral or neuraxial blocks are not an option, wound infiltration may provide some benefit especially when included as part of an overall perioperative MMA strategy.
For TKA, local anesthetics and other medications may be injected directly around the joint to improve pain control with or without the addition of peripheral nerve blocks although the combination of the two may be advantageous [44,45]. Periarticular infiltration analgesia may be comparable to femoral nerve block for the first 48 h after TKA, although femoral nerve block reduces opioid consumption to a greater degree [46]. Periarticular multimodal ‘cocktails’ typically consist of a dilute local anesthetic in addition to medications such as NSAIDs, epinephrine, and opioids [47,48]. While local anesthetic infiltration is commonly performed by surgeons [49], a newer ultrasound-guided technique known as the IPACK (infiltration between the popliteal artery and the capsule of the knee) facilitates performance by the anesthesiologist [50].
Intravenous local anesthetics
Intravenous local anesthetics, specifically lidocaine, may have a role in MMA protocols as well as Enhanced Recovery after Surgery (ERAS) protocols. Limited evidence suggests that lidocaine infusions reduce pain and opioid consumption as well as expedite return of bowel function after abdominal surgery [51] and analgesia during the first 48 h after spine surgery [52]. A meta-analysis in breast surgery found that acute postoperative pain was not improved with lidocaine infusions, but the risk of developing persistent postsurgical pain was reduced [53]. However, inclusion of a small number of studies limits this review. Lidocaine attenuates a number of pro-inflammatory molecules [54], and this is one proposed mechanism for its perioperative analgesic effects. As a generic drug, it is not expensive and should be considered as a component of ERAS protocols for abdominal surgery if epidural analgesia is contraindicated or not desired [55].
Opioid analgesics
Opioids have long been the standard perioperative analgesics of choice, a trend largely based on their simplicity, predictability, and familiarity. However, in light of the current opioid epidemic and greater awareness of opioid-related adverse events, attention has shifted from opioids to non-opioid analgesics as the foundation for perioperative pain management. The concept of reserving opioids for moderate or severe pain after alternatives have failed is not new and in fact was a cornerstone of the World Health Organization’s analgesic ladder that was first proposed in 1986 then recently updated with renewed emphasis on non-opioids as first-line for non-cancer pain [56]. As recent data reveal, MMA protocols for total joint arthroplasty (TJA) continue to include opioids as a component [57], and they are unlikely to be eliminated completely from the perioperative experience. However, the ever-expanding array of non-opioid agents has deepened the clinical armamentarium and given perioperative physicians the ability to minimize opioid exposure. Commonly used oral perioperative opioids include hydrocodone, oxycodone, and tramadol. Hydrocodone exists in several combination formulations and oxycodone is produced both in combination with acetaminophen and alone. Although commonly viewed as less likely to be abused because of its lower μ-opioid receptor affinity, tramadol has been highlighted in a 2017 report by the Centers for Disease Control and Prevention (CDC) for its association with long-term opioid use as well as a recent spike in emergency room visits [58]. Therefore, substituting tramadol for other opioids after surgery is likely not a significant improvement in safety or addiction potential.
Multimodal Analgesia, the Opioid Epidemic, and the Crisis of Drug Shortages
Evidence is accumulating that the risk of long-term opioid use after surgery increases with the length of initial prescription. Sun et al. [59] have reported that the risk of chronic opioid use in opioid-naïve patients after surgery is increased compared to that of non-surgical patients. In 8 of the 12 surgery types studied, including TKA, patients have an increased risk of filling either 10 or more prescriptions or more than 120 days’ worth, excluding the first 90 days. Brummett et al. [60] have also studied opioid-naïve patients who underwent a variety of surgeries, excluding orthopedic surgery, and similarly report an elevated risk among all surgical patients for long-term opioid use (defined as a prescription filled between 90 and 180 days). Interestingly, their reported rates of chronic use do not vary between minor and major surgical procedures. At the same time, the CDC has warned that the risk of long-term opioid use spikes at both 5 and 30 days in the initial prescription window [58]. Given the risk of long-term use that surgery itself introduces combined with the risk associated with prescriptions beyond a few days, efforts to reduce unnecessary opioid prescribing are warranted and already underway. Certainly, much of the focus is on opioid prescribing patterns, which we will not discuss here, but the implementation of MMA into routine perioperative care whenever possible is a step in the right direction.
Hebl et al. [11] have demonstrated that a TKA MMA protocol featuring a peripheral nerve block can produce meaningful benefits including decreases in length of stay and decreased opioid consumption. A large database study in patients who underwent TJA reports that, with each non-opioid agent added to a perioperative multimodal regimen, patients show a stepwise decrease in opioid consumption, opioid prescriptions, and length of stay [57]. Similar patterns have been noted outside of TJA as well. In a study of minor aesthetic plastic surgery procedures, switching from an opioid-based strategy to a non-opioid one does not compromise analgesia but does reduce nausea and vomiting and recovery time [61].
The concept of opioid-free surgery has been introduced and trialed at select institutions, although overall adoption has been slow and inconsistent [62]. Some proposed indications for opioid-free surgery include obesity, obstructive sleep apnea, chronic obstructive pulmonary disease, complex regional pain syndrome, cancer, and opioid tolerance [63]. Although conceptually it is logical that opioid-free surgery would reduce opioid-related complications and improve the perioperative patient experience, few outcome data have been published. When incorporated into an ERAS protocol, opioid-free surgery does not significantly reduce opioid prescribing patterns at discharge, even when pain scores and opioid use are low prior to discharge [64]. Clearly, there is still work to be done in determining the effect of opioid-free surgery on important outcomes and then accomplishing that goal in clinical practice. Any efforts to this end will rely heavily on MMA.
An additional challenge in managing perioperative pain today is that of ongoing drug shortages. Virtually every hospital and practice in the US has experienced this to some degree in recent years, and it can significantly alter a patient’s treatment. The causes of drug shortages are multifactorial and include quality and regulatory issues, company decisions to change strategy or discontinue manufacturing of a drug, or a shortage of raw materials [65]. Because three pharmaceutical companies manufacture 70% of the injectable medications used in the US and some perioperative medications are almost exclusively made by one company [65], shortages can have major, far-reaching effects on MMA strategies. Creating protocols that have some flexibility, such as substituting gabapentin for pregabalin or using alternative NSAIDs if one is not available, will prevent entire classes of drugs from being omitted in the perioperative period. This may not always be possible for agents with unique mechanisms of action, but for others it gives prescribing clinicians some options.
Anesthesiologists must also be creative at times when preferred drugs are not available and may need to turn to older drugs that are no longer commonly used. In one example from Canada, the local anesthetic chloroprocaine, a short-acting agent suitable for shorter procedures that was developed decades ago, was not readily available because of a lack of regulatory approval; anesthesiologists turned to prilocaine, an alternative intermediate-acting local anesthetic [66]. Although a lack of clinical studies comparing prilocaine to the more commonly used ropivacaine initially impeded its use, eventually studies were performed that justified the production and use of the older drug prilocaine [66]. This example may be particularly relevant for other generic drugs that are produced by one or a limited number of companies. Reliance on a single agent in any drug class used in perioperative pain management is no longer acceptable now that drug shortages are so common, and additional clinical studies of alternative drugs are needed to support their use. All anesthesiologists must develop a strong working relationship with their pharmacy colleagues in every practice location to develop a solid plan in terms of medication supply and alternatives in this era of frequent drug shortages so patients can continue to receive consistently high quality pain management in the perioperative period. Longer term solutions will require the involvement of professional societies and engagement of legislators.
Conclusions
In summary, evidence today supports the routine use of multimodal analgesia in the perioperative period to eliminate the over-reliance on opioids for pain control and to reduce opioid-related adverse events. A multimodal analgesic protocol should be surgery-specific, functioning more like a checklist than a recipe, with options to tailor to the individual patient. Elements of this protocol may include opioids, non-opioid systemic analgesics like acetaminophen, NSAIDs, gabapentinoids, ketamine, and local anesthetics administered by infiltration, regional block, or the intravenous route. While implementation of multimodal analgesic protocols perioperatively is recommended as an intervention to decrease the prevalence of longterm opioid use following surgery, the concurrent crisis of drug shortages presents an additional challenge. Anesthesiologists and acute pain medicine specialists will need to advocate locally and nationally to ensure a steady supply of analgesic medications and in-class alternatives for their patients’ perioperative pain management.
Notes
Dr. Schwenk has received consulting fees from Avenue Therapeutics (New York, NY, USA). This company had no input into any aspect of the present project or manuscript. Dr. Mariano does not have any conflicts of interest to declare.