A case series on simultaneous liver and kidney transplantation: do we need intraoperative renal replacement therapy?
Article information
Abstract
Since the implementation of the model for end-stage liver disease (MELD) scoring system in 2002, the liver transplantation (LT) society has observed a substantial increase in the number of recipients with renal dysfunction. Intraoperative renal replacement therapy (ioRRT) has emerged as one of the solutions available to manage high-MELD score recipients; however, its usefulness has not yet been proven. To date, we have experienced five cases of simultaneous liver and kidney transplantation (SLKT). Recipients of SLKT tend to have a lower pre-transplant kidney function and the longer operation time mandates a larger amount of fluid than LT alone. Hence, anesthetic care is more prone to be challenged by hyperkalemia, metabolic acidosis, and volume overload, making ioRRT a theoretically valuable intervention. However, in all five cases, recipients were managed without ioRRT, resulting in excellent graft and patient survival. As such, in this case series, we discuss current issues about ioRRT and SLKT.
In the United States (US), since the implementation of the model for end-stage liver disease (MELD) scoring system in 2002, there has been a substantial increase in the number of liver transplantation (LT) candidates simultaneously suffering from renal dysfunction [1]. To deal with these high-MELD score recipients with pre-transplant renal dysfunction, some transplantation centers in the US have started to incorporate intraoperative renal replacement therapy (ioRRT). Unfortunately, a significant amount of strong evidence validating the usefulness of ioRRT during LT is scarce. In Korea, LT candidate prioritization changed from the Child Turcotte Pugh scoring system to the MELD scoring system in June 2016. Accordingly, as it has been shown in the US, the number of LT recipients having pretransplant renal dysfunction will likely rapidly increase. Consequently, increasing cases of intraoperative complications, including hyperkalemia, metabolic acidosis, and volume overload are expected during LT. Additionally, decisions regarding the need for ioRRT will be addressed more frequently to anesthesiologists. As such, it seems to be a reasonable moment to retrospectively discuss our current state and to prepare for post-MELD era challenges.
Currently, our institutional strategy does not include the performance of ioRRT due to its lack of supporting evidence. We have managed over 1,700 cases of LT without ioRRT to date. Although there is a strong expectation that ioRRT would be beneficial for recipients with pre-transplant renal dysfunction, there is little evidence supporting the decision to accept ioRRT as a routine practice. Theoretically, simultaneous liver and kidney transplantation (SLKT) recipients are more suitable candidates for ioRRT than those undergoing LT alone, as recipients of SLKT have irreversible kidney disease that is not expected to improve following LT without the assistance of a kidney transplant (KT) procedure. In addition, patients undergoing SLKT experience a longer operation time and require a larger amount of fluids. Therefore, we felt it was beneficial to gather relevant SLKT cases and analyze them with respect to the inclusion of intraoperative renal dysfunction management. Discussions on ioRRT and SLKT will follow.
Case Report
Five cases of SLKT have been performed in our institute since our first LT procedure in 1996. Four recipients had end-stage liver disease due to hepatitis B virus, and one recipient had cryptogenic liver failure. Patients' MELD scores ranged from 21 to 23. Two recipients had hyponatremia preoperatively, and one recipient was managed in the intensive care unit (ICU) before the operation, but the patient did not require vasoactive drugs or ventilator therapy. None of the patients who underwent SLKT at our institute showed hepatorenal syndrome or encephalopathy prior to the operation.
In addition to liver disease, all of the five patients had renal dysfunction. Three had diabetic chronic kidney disease and one had membranoproliferative glomerulonephritis. The remaining one had unspecified glomerulonephritis and received KT in 2005, though the transplanted kidney became dysfunctional when he was hospitalized for the SLKT. All of the patients showed heterogeneity in kidney pathology, but none were expected to recover without a KT. Three of the patients had received preoperative renal replacement therapy (RRT), two via hemodialysis, and one via peritoneal dialysis. Kidney function assessed by serum creatinine (SCr)-based estimated glomerular filtration rate (eGFR) ranged from 3 to 46 ml/min. All SCr values were obtained before RRT. These three recipients received preoperative RRT a day before the scheduled operation. Additional detailed information of the recipients is shown in Table 1.
Operational procedures
During the SLKT procedures, we focused on keeping not only adequate blood pressure without volume overload, but also homeostasis of the acid-base, electrolytes, and coagulation system. First, intravenous fluids comprised of both crystalloids and colloids were infused, targeting a mean arterial pressure over 70 mmHg. In cases C and D, 0.9% saline was mainly infused while in case A, plasma solution A was mainly infused, as we changed maintenance fluid during LT from 0.9% saline to Plasma solution A (CJ Healthcare, Seoul, Korea). In cases B and E, the recipients had hyponatremia (124 mEq/L and 129 mEq/L, respectively) and so, 0.45% saline was the main fluid administered during the operations to prevent central pontine myelinolysis [2]. A continuous infusion of dopamine, norepinephrine, and vasopressin was also an effective option to maintain the target blood pressure. A large caliber central line (AVA, Edwards, Irvine, CA, USA) and pulmonary arterial catheter (Swan Ganz SvO2, Edwards, Irvine, CA, USA), with the aid of a corresponding monitoring system (Vigilance II, Edwards, Irvine, CA, USA), were utilized to choose the appropriate fluid and drug infusion rate.
Second, any imbalances of acid-base and electrolytes were monitored and corrected immediately. We performed arterial blood gas analysis from the start of operation and once every hour. A complete blood cell count, determination of international normalized ratio of prothrombin time (PT INR), activated partial thromboplastin time, fibrinogen, and thromboelastography were performed every two hours. At the start of both the anhepatic and the reperfusion phases, we set the clock to zero and recounted the time. Additional blood samples were collected at 10 minutes pre-reperfusion, and 5 and 30 minutes post-reperfusion. Ionized calcium values, below 0.8 mmol/L, were handled with 300 mg of calcium chloride. Potassium values over 4.5 mEq/L in pre-reperfusion period were handled with 10 international units (IU) or 5 IUs of regular insulin (RI) boluses, followed by a 5% dextrose solution infusion. To deal with metabolic acidosis, we infused 1 liter of 0.45% saline containing 80 mEq of sodium bicarbonate in cases in which base excess (BE) was below −10 mmol/L. However, in the first case (case E), we used a lower BE value to initiate bicarbonate infusion than that we use today [3].
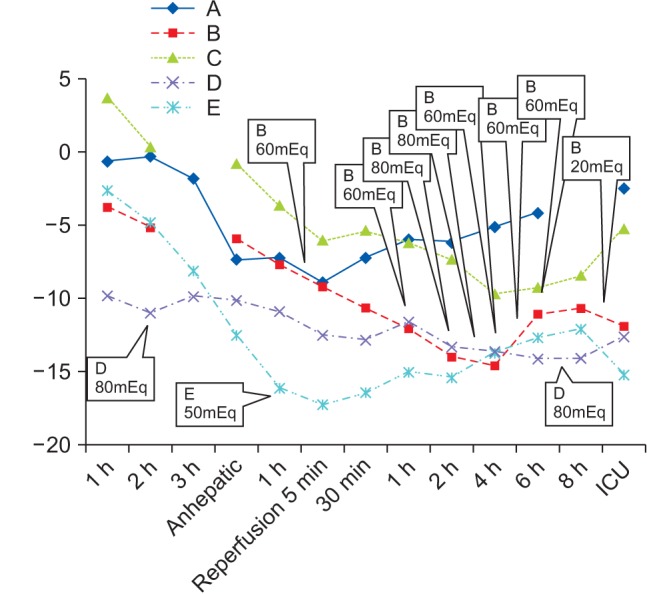
Lastly, a strict rule was applied to every decision involving blood product transfusion. In total, 300 ml of Cell Saver® (Haemonetics, Braintree, MA, USA) blood was infused in cases in which hemoglobin (Hb) was below 9 g/dl, and two units of leukocyte-depleted red blood cells (LDRBC) were infused in cases in which Hb was below 8 g/dl. Additionally, we prepared two units of fresh frozen plasma (FFP) for when PT INR was above 3 and one unit of single-donor platelet for when platelet count was below 30,000 /µl. Also, we infused six units of cryoprecipitates in cases in which fibrinogen was below 80 mg/dl, but only three units of cryoprecipitates when platelet count was above 50,000 /µl, even if the fibrinogen was below 80 mg/dl. Operation time as well as total input and output are shown in Table 2. The most extreme results of the potassium and BE interventions we carried out are shown in Table 3. Figs. 1 and 2 are time series plots demonstrating the results of the laboratory tests and interventions.

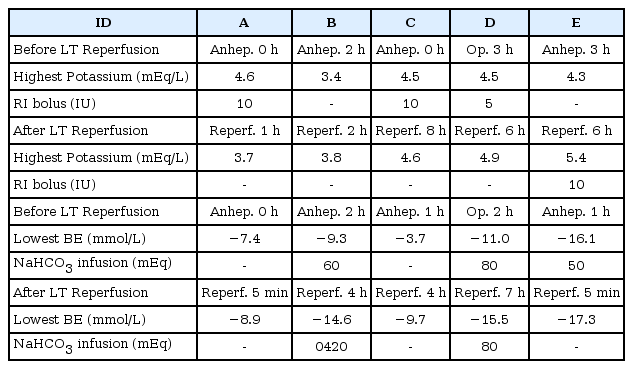
Results of Potassium and Interventions Followed. In all cases, insulin bolus therapy was carried out to keep the potassium value under 4.5 mEq/L in pre-reperfusion period, and 5 mEq/L in post-reperfusion period. In case A, C, and D, each needed one insulin bolus in pre-reperfusion period. In case E, two insulin boluses were needed in post-reperfusion period. ICU: intensive care unit.
Hyperkalemia and metabolic acidosis
In cases A, C, and D, one RI bolus was needed in each prereperfusion period (because potassium values were 4.6 mEq/L, 4.5 mEq/L, and 4.5 mEq/L, respectively). In case E, RI bolus was not required in the pre-reperfusion period, but two RI boluses were given in the post-reperfusion period (because potassium values were 5.4 mEq/L and 5.1 mEq/L, respectively). In case B, RI bolus was not required at any point throughout the operation.
In cases A and C, BE values were kept above −10 mmol/L, throughout the operation, and sodium bicarbonate infusion was not needed. In case D, 80 mEq of sodium bicarbonate was infused in the pre-reperfusion period (BE value was −11.0 mmol/L at two hours into the operation) and another 80 mEq of sodium bicarbonate was infused in the post-reperfusion period (BE value was −15.5 mmol/L at seven hours post-reperfusion). In case E, 50 mEq of sodium bicarbonate was infused in the pre-reperfusion period (BE value was −16.1 mmol/L at one hour into the anhepatic) but sodium bicarbonate was not followed even when the BE decreased to lower than −15 mmol/L in the post-reperfusion period. On the contrary, in case B, vigorous efforts to keep the BE above −10 mmol/L in both the pre- and post-reperfusion periods were carried out. A total amount of 480 mEq of sodium bicarbonate was infused as a result. Ironically, this patient, who received the most aggressive sodium bicarbonate therapy, died a month after the operation. He was the only recipient who received both deceased liver and kidney grafts, and also the only one who received continuous renal replacement therapy (CRRT) after the operation. Our aggressive sodium bicarbonate infusion therapy worked effectively throughout the operation. However, inappropriate function of the deceased liver and kidney grafts, to our knowledge, initiated the fatal clinical outcome in the post-operative period.
Metabolic acidosis was managed tightly in four of the cases (in cases A, B, C, and D). In case E, however, the BE value to initiate the infusion of sodium bicarbonate was lower than that we use today [3]. As a result, less aggressive sodium bicarbonate infusion therapy was conducted, and even a BE value below −15 mmol/L was observed without intervention. However, as the kidney graft successfully functioned, the laboratory results all converged to normal after the operation, and hemodynamic instability remained unreported during the operation.
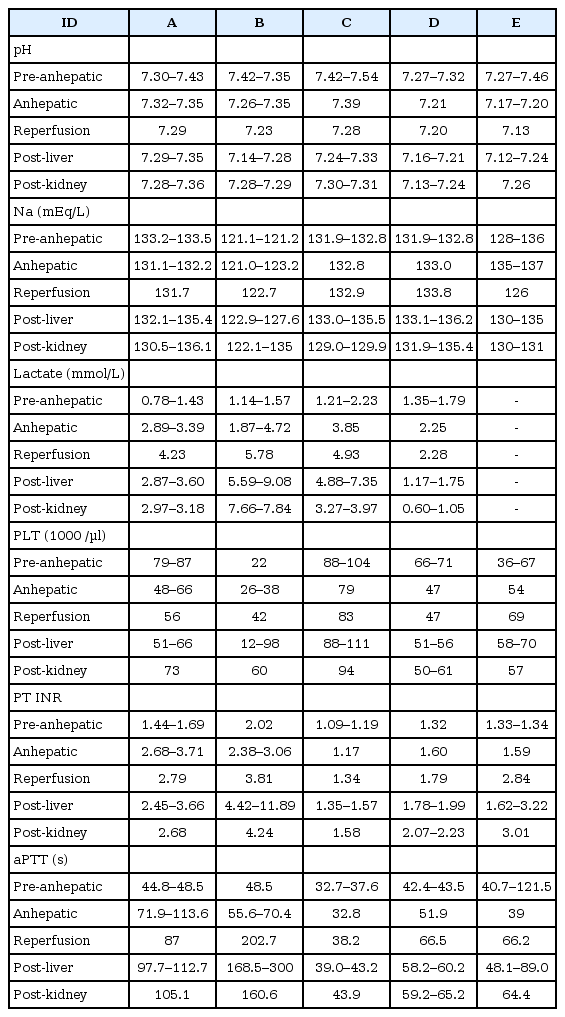
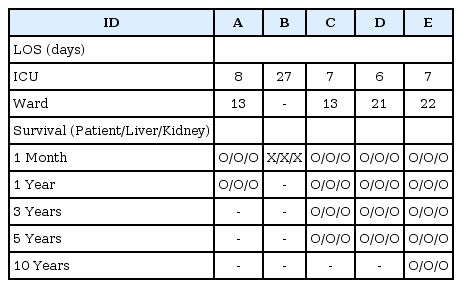
None of the five recipients showed signs or symptoms of volume overload in the post-operative period. Post-operative chest X-rays revealed absence of pulmonary edema and/or pleural effusion in all cases. The PaO2/FIO2 value before extubation a ICU was 254 (A), 361 (B), 418 (C), 263 (D) and 256 (E), respectively. Laboratory results other than potassium and BE during the operation are shown in Table 4, while laboratory results at ICU are shown in Table 5. Length of hospital stay, patients and grafts survival rates are shown in Table 6.
Accumulation of wasted materials
Even if potassium and metabolic acidosis were managed sufficiently without the use of ioRRT, it is unknown how much waste material is being accumulated during the operation. To identify it, in the most recent case (case A), we performed an additional laboratory test just before the reperfusion of the kidney graft. It took approximately 12 hours from the start of the operation to the reperfusion of the kidney graft. Blood urea nitrogen and SCr values before the operation were 17 mg/dl and 1.93 mg/dl respectively, and they decreased to 11.7 mg/dl and 1.31 mg/dl just before the kidney reperfusion. Total input and output at that moment were 15,100 ml of crystalloid, 1,670 ml of 5% albumin, 1,000 ml of 6% Hextend (CJ Healthcare, Seoul, Korea), 500 ml of 6% Volulyte (Fresenius Kabi, Bad Homburg, Germany), 430 ml of 15% mannitol, 1,439 ml of Cell Saver® blood, two units of LDRBC, four units of FFP, six units of cryoprecipitate, and 2,140 ml of urine output. Total estimated blood loss was 5,175 ml. We discussed the decrement of SCr during the operation and postulated that the decrement of body waste could be the result of the removal of a huge amount of body fluid via surgical bleeding. Meanwhile, supplementation of fluids and fresh blood products mimicked the function of ioRRT.
Discussion
In the Korean Journal of Anesthesiology, four case reports of SLKT were identified. In 2002, Lee et al. [4] reported a case of SLKT (living liver and kidney donor) in a 45-year-old man receiving preoperative hemodialysis. Authors discussed the case with transplant surgeons and decided not to use ioRRT because of its unfamiliarity. Instead, they decided to implant the kidney graft earlier and the liver graft later, to ease the intraoperative management of renal dysfunction. Liver grafting is usually implanted earlier than kidney grafting to avoid kidney graft hypoperfusion during the liver reperfusion period, and to shorten the ischemia time of liver grafting, which is known to be more more limited than that of the kidney grafting. However, the authors in that case concluded that in the living donor LT, ischemia time could be shortened by timing the operation of the donor to that of the recipient. The implanted kidney graft functioned well during whole operation, including in the liver reperfusion period, and anesthesia was maintained successfully.
In 2009, Park et al. [5] reported a case of SLKT (deceased liver and kidney donor) in a 13-year-old child receiving preoperative peritoneal dialysis. Authors found it difficult to place an additional large caliber central line in a child, and so did not use ioRRT. Instead, they used non-potassium-containing fluid, fresh blood products within a week and sodium bicarbonate infusion, which resulted in an adequate acid-base and electrolyte balance during the operation. Of interest in that case is the fact that the authors used non-potassium-containing 0.9% saline during SLKT. Recent studies on balanced crystalloids have revealed the benefits of low incidence of hyperchloremic metabolic acidosis and renal vasoconstriction, implicating less kidney injury [6]. In addition, a more recent randomized controlled study reported that the risk of hyperkalemia in KT recipients receiving acetate-buffered balanced solution was not significantly higher than in KT recipients receiving 0.9% saline, although the former solution contains potassium [8]. Therefore, in light of this information, we changed our primary fluid during LT and KT from 0.9% saline to acetate-buffered balanced crystalloid (i.e., Plasma solution A).
In 2002, Huh et al. [7] reported two cases of SLKT. One involved a deceased donor and the other involved a living donor. Authors used ioRRT in the living donor case, and a clot formation in the filter disabled the system two hours after initiation. They replaced the filter, and the system stopped again after another two hours. The last period of anesthesia was maintained well without ioRRT. Theoretically, ioRRT actually has several complications. Above all, ioRRT has a risk of filter clotting. Unfortunately, systemic anticoagulation has a risk of increased bleeding tendency. It is difficult to stay at an appropriate point between pro-coagulation and anti-coagulation in patients with end-stage liver disease because they already have a drifting balance of coagulation. Recently, a regional anticoagulation technique with circuit inborn citrate was invented as an alternative. Other reported complications of ioRRT include hypothermia, vascular access dysfunction, fluid and electrolyte balance errors and, rarely, mechanical problems. Financial issues should also not be ignored, because ioRRT has been reported to consume a significant portion of national medical insurance resources in Korea.
As a next step, we searched international reference databases and found a few studies on the use of ioRRT in LT and SLKT. In the early 2000s, there were sporadic case reports and experience reports prepared by a single center or authors with a small-sized study population, addressing the possibility of better intraoperative management of metabolic and acid-base homeostasis with ioRRT. In 2011, Parmar et al. [9] reported a retrospective cohort study of ioRRT in 72 LT recipients, and noted that there was no difference in post-operative complication rates between ioRRT and non-ioRRT groups, despite the fact that the ioRRT group had a higher pre-operative disease severity and CRRT ratio. However, this report was limited by the failure to incorporate matching between the two groups. In 2014, Agopian et al. [10] reported a retrospective cohort study of ioRRT in 407 LT and 93 SLKT recipients who were already receiving preoperative CRRT. Among them, 401 patients did not receive ioRRT, 70 patients received planned ioRRT, and 29 patients received emergent ioRRT. Perioperative variables were analyzed between these three groups, and the authors observed similar intraoperative complication rates between the planned-ioRRT group and non-ioRRT group, despite the fact that preoperative disease severity variables were significantly worse in the planned-ioRRT group. From this, they suggested that these intraoperative outcomes, observed to be better than expected in the planned-ioRRT group, were in fact due to the utilization of ioRRT. In addition, they observed significantly lower intraoperative complication rates in the planned-ioRRT group than in the emergent-ioRRT group, despite the fact that preoperative disease severity variables were similar in the two groups. From this, the authors also suggested that the inferior intraoperative results in the emergent-ioRRT group could be due to not initiating ioRRT as a planned intervention.
As was demonstrated, most studies on the use of ioRRT are mainly observational or retrospective, and the necessary strong evidence does not exist so far. Fortunately, according to clinicaltrials. gov, the first large multicenter, prospective randomized controlled trial is in process by Bagshaw et al., which began in 2012. This study is designed to compare ioRRT during LT with standard supportive therapy in patients with a glomerular filtration rate (GFR) of less than 60 ml/min. The results are preliminary and the study population is limited to non-pre-transplant CRRT patients receiving LT alone; nevertheless, the study may become a cornerstone for ioRRT research and may affect the future management of high-MELD score recipients in the future.
Simultaneous liver and kidney transplantation
As a last step in this study, we searched literature databases for SLKT listing criteria. We realized that almost all of the SLKT recipients in Korea, including the patients from our cases, showed lower MELD scores as compared with recipients in the US. In living donor SLKT, the availability of simultaneous donors exerts more leverage on the decision of SLKT than the nature of the disease itself. However, even in the deceased donor case (case B), kidney function was enough to filtrate body wastes without RRT (SCr 1.58 mg/dl). This may be attributed to the current non-existence of SLKT listing criteria in Korea. In the US, there are a few consensus guidelines on SLKT listing criteria, which have been largely made and revised using Organ Procurement and Transplantation Network (OPTN) data. However, they are, by all means, not perfect and there are still many obstacles to be solved.
First, currently there is no consensus on the definitions of AKI and chronic kidney disease (CKD) in the setting of LT. It is well known that SCr, the classic biomarker, can lead to overestimation of the true kidney function in end-stage liver disease recipients. However, the feasibility and widespread laboratory availability of SCr has made it to form the basis for estimating the degree of renal dysfunction, even in LT and SLKT. For now, the most notable definition of renal dysfunction is the Risk, Injury, Failure, Loss, End-stage kidney disease (RIFLE) 5 stage criteria developed in 2004, which was modified to a three-stage system by the Acute Kidney Injury Network (AKIN) in 2007. Kidney Disease: Improving Global Outcomes (KDIGO) in 2012 added a last touch to the RIFLE criteria by formulating albuminuria criteria and applying a time frame to the SCr criteria. Furthermore, to define renal dysfunction in LT recipients, a working party by the Acute Dialysis Quality Initiative (ADQI) and International Ascites Club in 2011 suggested a proposal to apply the RIFLE criteria to define AKI and CKD in patients with cirrhosis, irrespective of the cause [11]. New candidates for biomarkers, such as cystatin C and neutrophil gelatinase-associated lipocalin (NGAL), are currently under investigation. A new definition of renal dysfunction made up by those novel biomarkers is needed to create an appropriate SLKT listing criteria.
Second, key factors that determine non-recovery of kidney function after LT remain poorly defined. Recently, Sharma et al. [12] reported a retrospective review analyzing 2,112 adult deceased donor LT recipients who received acute RRT for less than 90 days before LT. The authors concluded that native renal function was recovered in the majority of patients within six months post-transplant, with the cumulative risk of renal non-recovery being 8.9%. According to the study by Sharma et al., risk factors of renal non-recovery were age at LT, longer duration of RRT, retransplant and pre-LT diabetes. Although it is a good option for a patient who has both end-stage liver and kidney disease, SLKT should not be performed in patients in whom renal dysfunction is expected to disappear after LT. According to literatures, in the past decade in the US, more than 30,000 adults were added to the KT waiting list annually, but only 55–60% eventually received a deceased kidney graft. During that same time period, 13–15% of the individuals on the waiting list died while waiting for a transplant and 3–10% of them were removed from the list due to high disease severity. It should be noted that organ shortage is apparent in Korea, too. Further research on eligible risk factors is needed to avoid overzealous listing for SLKT.
Third, the appropriate time to initiate RRT in recipients waiting for SLKT is unknown. In the first national survey of practice patterns of SLKT in the US by OPTN, 70% of centers used dialysis duration as a criterion to determine the need for SLKT, whereas 30% of centers used AKI duration [1]. However, there is still no guideline regarding when to start RRT in recipients waiting on a list. The decision of when to begin RRT is especially difficult to make in cases in which recipients develop AKI. Thus, a consensus on this decision is essential to build an acting SLKT criteria that embodies all recipients with or without RRT.
Lastly, there are debates regarding the true benefits of SLKT. In a review based on OPTN data by Formica et al. [13], recipients undergoing LT with SCr > 2.5 mg/dl or pre-transplant dialysis time of > 2 months have 81.1% one-year survival rate and 65.9% five-year survival rate. SLKT increased this outcome to only 86.2% and 70.1%, respectively. More recent study data based on a propensity score-analysis of OPTN data concluded that survival benefit may even be as little as one month at five years after transplantation [14]. In addition, transplantation of a kidney graft in recipients of LT with a high risk of mortality can be a waste of scarce organs. In a single-center study consisting of 169 patients with a MELD score > 40, futile LT outcomes (defined as three-month mortality or in-hospital mortality) occurred in over 22% of those involved in the study. In another analysis using the national database, patients with MELD score > 40 were more than twice as likely to die within 30 days of transplant than those with MELD scores of less than 30. According to them, futility predictive factors included age > 60 years, body mass index > 30 kg/m2, a pre-transplant requirement for ICU care or life support and the presence of multiple comorbidities [15]. The overall one-year kidney graft survival after SLKT was 77.2%, while graft survival after KT alone was 89.3%, following OPTN data in a similar study. Thus, the additory benefit from SLKT over LT alone should be better estimated and balanced with the disadvantage of patients waiting for KT alone.
Despite all of the limitations above, several consensus guidelines for SLKT listing criteria were made and published by several researchers as well as associations and government divisions in the US. The most notable ones are those from two big consensus conferences by OPTN. The first one was published by Eason et al. in 2008 and the second one by Nadim et al. in 2012 [1]. The latter one adopted and modified the definition of AKI and CKD by KDIGO, and consisted of persistent AKI for more than four weeks, CKD for three months and metabolic diseases that affect both the liver and kidney. Recently, OPTN pronounced a new SLKT allocation criteria in 2016 [13]. Those criteria are as follows. Metabolic diseases requiring SLKT (for example, primary hyperoxaluria), sustained AKI (defined as eGFR < 25 ml/min for six consecutive weeks) and/or CKD (defined as eGFR < 60 ml/min for> 90 days prior to listing and < 30 ml/min at the time of listing). All eGFR values are based on a six-variable Modified Diet in Renal Disease (MDRD6) formula. The guideline in 2016 also incorporated the concept of a “safety net,” which means prioritizing the patients who received LT to the kidney graft listing, in case of renal non-recovery. It was suggested that the addition of this component may affect the decision to undergo SLKT by removing the concern that if a patient does not receive the SLKT, that they will remain on dialysis and suffer a worse outcome.
In summary, we searched reported references to figure out the necessity of ioRRT in LT and SLKT. We also searched references to make an appropriate decision on the performance of SLKT, instead of LT alone. As we discussed above, great challenges are expected following the adoption of the MELD scoring system. It is not just a simple matter of increasing renal dysfunction; there are bundles of problems to be solved, like a domino effect. Utilization of novel biomarkers in LT recipients, the development of a more precise formula to detect kidney injury earlier; locating more risk factors on post-LT renal non-recovery; analyzing the effects of ioRRT on the renal recovery and determining the benefits of ioRRT in either living or deceased grafts; investigating complication reports of ioRRT; building a national statistics of SLKT and ioRRT; estimating the additory benefit from SLKT and the disadvantage of patients on KT waiting list; and finally, establishing our own consensus criteria for both ioRRT and SLKT are all important considerations in the post-MELD era of LT anesthetic portion of care. Further research is needed indeed in next decade.