Introduction
As a non-depolarizing muscle relaxant, rocuronium is useful for endotracheal intubation due to rapid onset time, but it produces injection pain, which is often associated with withdrawal movement of the injected hand or arm, in 50-80% of injected patients [
1]. Even in unconsciousness patients administered with anesthetic induction agents, rocuronium causes withdrawal movement, indicating intense pain [
2]. Therefore, a variety of pretreatments have been attempted to reduce the rocuronium injection pain. Turan et al. [
3] demonstrated that a small dose of magnesium, average 7 mg/kg, reduced rocuronium injection pain effectively compared to lidocaine, sodium bicarbonate and alfentanil.
As a calcium channel blocker and a physiological antagonist of the N-methyl-D-aspartate (NMDA) receptors magnesium has reduced the anesthetic requirement during surgery and analgesics for postoperative pain control [
4-
7]. Although the exact mechanism is not clear, magnesium was also demonstrated to have a local analgesic effect in reducing injection pain by intravenous propofol [
8,
9] and rocuronium [
3].
After muscle relaxation with rocuronium, subsequent laryngoscopy and tracheal intubation (LTI) causes inevitable hemodynamic changes such as hypertension and tachycardia. Magnesium has also been suggested as a useful strategy in attenuating the adrenergic response to LTI [
10,
11]. However, in those studies, the authors used 50 or 60 mg/kg of magnesium to attenuate the hemodynamic response to LTI. That dose was much larger than the required amount of magnesium to reduce rocuronium injection pain. To date, few studies have investigated the effective doses of magnesium, which can attenuate both rocuronium injection pain and the following hemodynamic responses by LTI in general anesthesia.
Therefore, the aim of this study was to evaluate the effectiveness of pretreatment with magnesium using doses of 5, 10, and 20 mg/kg for both the prevention of rocuronium injection pain and the attenuation of the resulting hemodynamic response after LTI.
Materials and Methods
After obtaining our institutional ethics committee approval and patients' written informed consent from each patient, 200 America Society of Anesthesiologists physical status classification (ASA) I-II patients undergoing various elective surgeries with general anesthesia were randomly divided to 4 groups (all n = 50). They received normal saline 5 ml (group 1), magnesium sulfate 5, 10 and 20 mg/kg (groups 2, 3 and 4), respectively, before rocuronium injection. To attenuate hemodynamic stimulation, 20 mg of esmolol (methyl 3-4-[2-hydroxy-3-(isopropylamino) propoxyphenyl] propionate hydrochloride) was given to group 1 before LTI. Randomization was conducted by computer-generated codes that were maintained in sequentially numbered envelopes. Exclusion criteria were prior use of calcium channel blockers, opioids and anticoagulants, pregnancy, known allergy to magnesium sulfate, disorders of cardiovascular, hepatic, renal, gastrointestinal and neurological diseases, morbid obesity, and difficult airway. No premedication was given to any patients. Before the induction of anesthesia standard monitoring of heart rate, non-invasive arterial pressure, ECG and arterial oxygen saturation was initiated. All patients had an 18 gauge IV catheter on the forearm and all drugs were administered near the IV catheter. Anesthesia was induced with propofol (2 mg/kg). After finding the abolished eyelid reflex, either normal saline 5 ml, or magnesium sulfate (5, 10, or 20 mg/kg) prior to 0.6 mg/kg of rocuronium was administered over one minute according to the assigned groups. Intravenous fluid infusion was occluded for 30 seconds after magnesium injection in all groups. Mask ventilation with sevoflurane in 100% oxygen was maintained for 90 seconds after rocuronium injection, before LTI. Anesthesia after LTI was maintained with an end tidal sevoflurane concentration of 2-2.5% in a mixture of air and oxygen 50%.
The patient's response, as feeling of pain or discomfort, to intravenous rocuronium injection was assessed by observing patient's movements, such as no movement (grade 0), movement only wrist (grade 1), movement to the upper arm and shoulder of injected arm (grade 2) or generalized movements (grade 3).
Hemodynamic variables such as systolic and diastolic blood pressure (SBP and DBP) and heart rate (HR) were recorded before the anesthetic induction (baseline value), before and 1 min after tracheal intubation.
Data are expressed as means ± standard deviation (SD) or numbers of patients (percentages). Chi-square test or Fisher's exact test was used for sex ratio and degree of withdrawal movements during injection of rocuronium among the groups. One way analysis of variance (ANOVA) for age, weight and height. A mixed linear model with Bonferroni's correction within the groups and ANOVA with Bonferroni's correction among the groups for hemodynamic changes at all study stages, were used. P < 0.05 was considered statistically significant.
Results
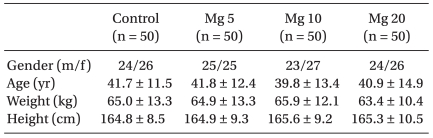
The demographic data were comparable among all groups (
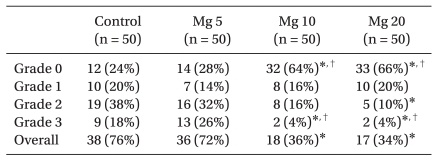
Table 1). Administration of magnesium at 10 and 20 mg/kg significantly reduced the incidence of overall movement compared to the saline control after rocuronium administration (34% and 36% in the group 3 and 4, respectively vs. 76% in group 1) (P < 0.0001, for both comparisons). Withdrawal movement (grade 3), indicating severe pain, was seen in 4% of patients in both the magnesium 20 mg/kg and 10 mg/kg groups, respectively (both groups vs. saline, P < 0.05; both groups vs. magnesium 5 mg/kg, P < 0.05) (
Table 2).
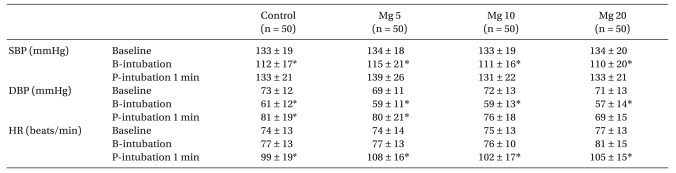
The mean baseline values for SBP, DBP and HR were comparable among the groups (
Table 3). The SBP and DBP values following anesthetic induction before intubation were significantly lower compared to baseline values within the groups (P < 0.001 in each group). LTI caused no increase of SBP and DBP with the administration of magnesium sulfate at 10 mg/kg or 20 mg/kg prior to intubation, but significant increases in DBP were seen with administration of esmolol (20 mg) or magnesium sulfate (5 mg/kg) compared to baseline values within each groups (P < 0.001). During anesthetic induction, HR was not different compared to baseline value within the groups. LTI caused a significant increase in HR compared to baseline values in all groups. Adverse effects such as severe hypotension or bradycardia was not seen in any patients following administration of either esmolol or magnesium at any doses before LTI. Although magnesium may potentiate neuromuscular blockade, it was assumed that the administration of magnesium sulfate (5, 10 or 20 mg/kg) did not prolong muscular relaxation in this study, because no patient was delayed to resume of ventilation at the end of surgery.
Discussion
In this study, we found that intravenous pretreatment with 10 or 20 mg/kg of magnesium prior to rocuronium administration significantly alleviated rocuronium injection pain, 20 mg/kg better than 10 mg/kg. In addition, magnesium at 10 or 20 mg/kg prior to rocuronium provided stable blood pressures immediately after LTI.
Rocuronium is an attractive muscle relaxant due to rapid onset of action, and it works as fast as succinylcholine. However, high incidence of hand or limb withdrawal or generalized movement is seen, indicating injection pain, even under anesthesia, which can be a considerable drawback for rocuronium. The mechanism by which rocuronium causes injection pain is speculative [
12,
13]. Therefore, to overcome rocuronium induced withdrawal movement, a various studies using different drugs have been investigated [
12,
14-
16]. In this study, 10 and 20 mg/kg of magnesium significantly reduced the overall incidence of movements associated with intravenous rocuronium, when compared to the saline control group. Generalized movement, indicating severe pain, was found only in 4% of patients administered magnesium at 10 or 20 mg/kg.
Magnesium sulfate, known to be a natural calcium channel blocker, has shown to have antinociceptive effects via inhibition of calcium channels and NMDA receptors [
5]. Therefore, magnesium has been considered as a useful anesthetic adjunct for intra- and postoperative analgesia in anesthetic practice [
4,
6,
7]. The local analgesic effect of magnesium has also been suggested in previous studies. For example, magnesium reduced local injection pain associated with intravenous propofol [
8,
9] and rocuronium [
3]. Agarwal et al. [
8] suggested that pretreatment with 1 g of magnesium minimized propofol induced pain and was as effective as 40 mg of lidocaine. In another comparison study aiming to prevent the injection pain by rocuronium, 2 ml of 2.48 mmol magnesium was found to be as effective as 30 mg of lignocaine, 2 ml of 8.4% sodium bicarbonate or 1,000 µg of alfentanil [
3]. However, since it has been suggested that pretreatment with magnesium itself causes pain [
8], caution for slow administration of magnesium may be needed. But, administration of magnesium sulfate over one minute in this study did not demonstrate any pain on injection per se as well as circulatory collapse.
LTI after intubating dose of rocuronium produces marked increase in BP and HR due to catecholamine release. Because hemodynamic changes by LTI may be associated with serious medical conditions, various techniques including administration of magnesium, to attenuate the adrenergic responses by LTI have been investigated [
10,
11,
17]. Pretreatment with intravenous magnesium (40 mg/kg) was reported as a helpful adjunct in reducing hemodynamic responses after succinylcholine facilitated tracheal intubation [
17]. Further 60 mg of magnesium sulfate effectively attenuated the catecholamine release and hemodynamic response after non-depolarizing muscle relaxant induced LTI [
10]. In compromised patients with coronary artery disease, magnesium at 50 mg/kg before the induction of anesthesia resulted in stable hemodynamic responses to LTI compared to lidocaine [
11]. In the current study, administration of magnesium (10 or 20 mg/kg) prior to rocuronium to alleviate rocuronium injection pain also prevented the increase in blood pressure immediately after LTI. However, the significant increase in HR after LTI was not prevented with 10 or 20 mg/kg of magnesium administration. Therefore, further studies to find the optimum dose of magnesium prior to rocuronium for inhibiting both rocuronium injection pain and the hemodynamic changes following LTI is needed. As a standard regimen to reduce hemodynamic changes by LTI in the control group, we used i.v. esmolol (20 mg) immediately before LTI [
18]. A larger dose of esmolol was more effective in minimizing LTI induced responses, but it also showed a potential risk for severe bradycardia and hypotension in a low stress condition [
19]. Therefore, we chose 20 mg of esmolol before LTI as a dose that would prevent severe hypertension and tachycardia without inducing significant hypotension and bradycardia.
In conclusion, although a dose that controlled both the pain related to rocuronium and the hemodynamic responses to intubation was not determined in this study, we found doses of magnesium (10 and 20 mg/kg) that alleviated the pain associated with rocuronium injection and as well as the changes in blood pressure after LTI.